Understanding the symptoms of MS
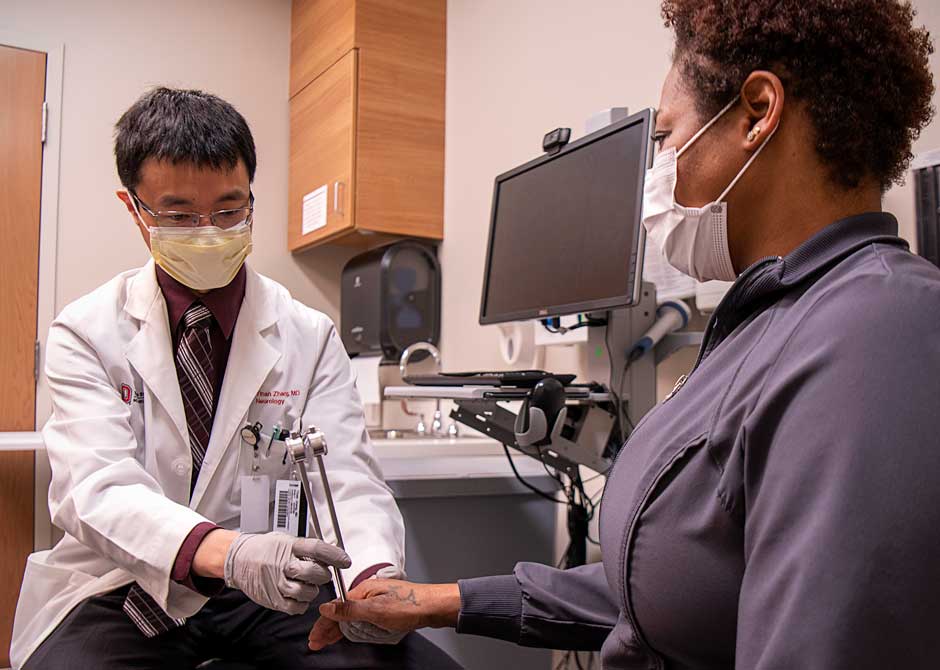 Because multiple sclerosis (MS) attacks the central nervous system, it can cause a range of challenges that vary widely from person to person. The most fortunate patients have only mild symptoms, while others struggle with bigger interruptions to their life. The first symptoms may be vague, and many of the symptoms can be caused by conditions other than MS.
Because multiple sclerosis (MS) attacks the central nervous system, it can cause a range of challenges that vary widely from person to person. The most fortunate patients have only mild symptoms, while others struggle with bigger interruptions to their life. The first symptoms may be vague, and many of the symptoms can be caused by conditions other than MS.
Symptoms depend on which parts of the central nervous system have been damaged and the extent of that damage.
The length of time you have individual symptoms may vary too. They may last from days to months and then wane or resolve (relapsing-remitting) or persist and slowly worsen over time. Some symptoms of MS are chronic, and fluctuate hour to hour, or day to day; the most common among these are fatigue, memory difficulties or muscle spasms. In addition, a rise in body temperature or an infection can sometimes cause old symptoms to reappear or worsen temporarily.
Common symptoms of MS include:
- Fatigue/feeling very tired – can occur even in the absence of sleep problems or can worsen as other symptoms make it hard to sleep.
- Muscle or motor symptoms – weakness in one or more limbs; foot drop/leg dragging; stiffness and cramping of the muscles (spasticity); weak hand grip; a feeling of leg heaviness.
- Vision or eye problems – blurred, foggy or hazy vision in one or both eyes; dulled color vision; pain behind, or at the corner of, an eye (often triggered by eye movement); blindness; double vision. Optic neuritis — diminished vision in one eye that is often painful — is a fairly common first symptom of MS.
- Sensory symptoms – tingling; pins-and-needles sensations; numbness (a lack of feeling) in one or more limbs; a band of tightness around the chest or abdomen; burning pains or hypersensitivity to temperature or touch; stabbing facial pain; electrical sensations down the neck or back that are triggered by looking down.
- Difficulties with coordination or balance – unsteady walking and frequent falling; veering to one side; loss of hand/finger dexterity; deterioration of handwriting; vertigo (room spinning); tremor.
- Gait issues (uneven, difficult walking) – caused by loss of leg strength and balance issues.
- Bladder symptoms – inability to hold urine (urinary incontinence), completely empty the bladder or sense bladder fullness.
- Constipation and other bowel disorders
- Male erectile dysfunction (impotence) and female sexual dysfunction
- Difficulty with swallowing; choking on liquids or solids
- Slurred or uneven speech
- Cognitive and emotional problems – memory loss; difficulty with multitasking; uncontrollable crying or laughing. These are more common in people who’ve had MS for some time. Depression is more common among people with MS than in the general population.
How is MS diagnosed?
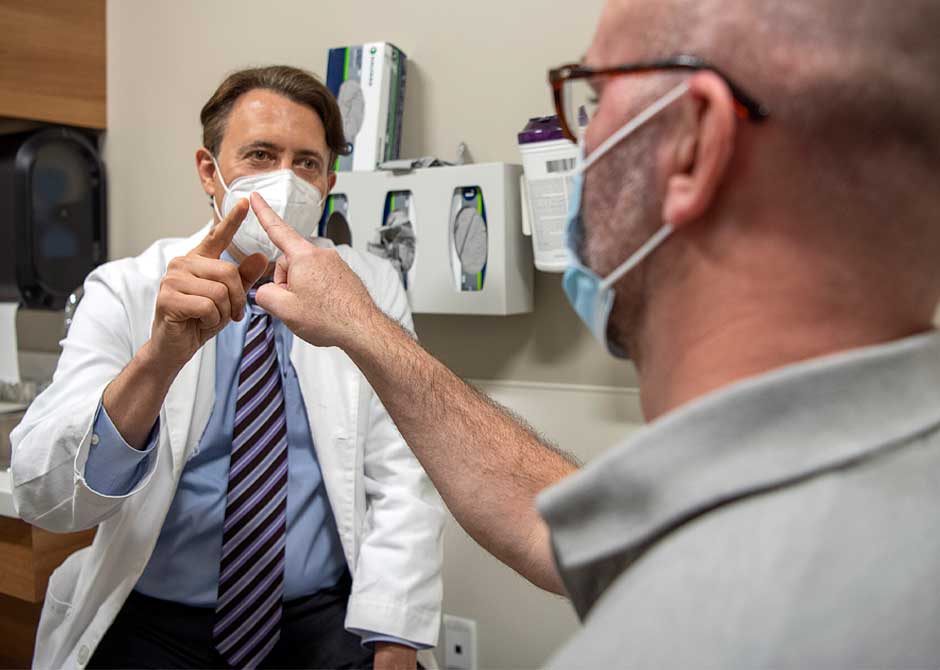
Diagnosing MS isn’t always easy and, in some cases, may take time. An accurate diagnosis is critical in creating an effective care plan.
Diagnosing relapsing-remitting MS (RMMS)
An important feature of RRMS is “dissemination (or separation) in space and time,” meaning there must be evidence of two or more lesions that developed at different locations in the central nervous system at different time points. A patient must have experienced at least one clinical attack for a definitive diagnosis to be made.
According to the most recent guidelines (called the McDonald criteria), the requirement for separation in time can be replaced by finding “oligoclonal bands” through a spinal tap test.
Diagnosing progressive MS
In contrast, progressive MS is characterized by a gradual neurological decline, with or without superimposed clinical relapses, along with the presence of typical MS lesions in the brain or spinal cord, as revealed on MRI scans. Alternative diagnoses must be ruled out. The doctor will examine you, ask you questions about your symptoms and do some tests. Tests may help confirm or rule out the diagnosis when your history and exam don’t provide enough information.
Tests used to diagnose MS
MRI (magnetic resonance imaging) is a common procedure that uses a magnetic field and radio waves to create detailed images of the brain and spinal cord. MRI is often used to confirm the diagnosis of MS, because the patches of damage (lesions) in the brain and spinal cord caused by MS attacks can be visualized using this technique. Even when inflammation subsides, a permanent scar is often left behind. MRI scans of the brain and different segments of the spinal cord are usually ordered individually. Scans may be done before and after administering a dye, called gadolinium, to highlight areas of active inflammation.
Blood tests check for vitamin deficiencies, infections and markers of alternative autoimmune diseases and inflammatory diseases of the central nervous system that cause symptoms that overlap with MS.
Lumbar puncture (spinal tap) can check spinal fluid for specific markers associated with MS. One important spinal fluid marker is called “oligoclonal bands,” which are inflammatory proteins present in the majority of individuals with MS.
Evoked potential tests measure the speed at which the brain tracks electrical signals in response to light, sound or touch stimuli. There are three types: visual evoked potentials measure signals triggered by watching an alternating checkerboard pattern; brainstem auditory evoked potentials measure signals triggered by a series of clicks in each ear; and sensory evoked potentials measure signals triggered by short electrical pulses on the arms or legs.
Optical coherence tomography (OCT) is an instrument that allows doctors to examine the retina (the lining at the back of the eye), which is often thinned in people with MS.
Tests used to diagnose health problems associated with MS
Urinary tests, such as a bladder ultrasound, may be needed to help determine the cause of bladder control difficulties in a person who has MS, and to aid with symptomatic management.
Neuropsychological tests may be necessary to diagnose thinking or emotional problems, which may be present without the person being aware of them. Typically, these tests follow a question-and-answer format.
Blood tests can gauge the likelihood of side effects from a potential disease-modifying drug, or a drug used to alleviate symptoms. Such tests may include blood cell counts, liver function tests and tests to determine immunity against (and susceptibility to) certain viral infections. For example, a blood test for exposure to the John Cunningham (JC) virus can help you and your doctor gauge the risk for getting a rare but serious brain infection called PML (progressive multifocal leukoencephalopathy) that’s more common in patients taking specific disease-modifying therapies. In addition, your blood may be taken to measure your serum vitamin D level, since there’s some evidence that low vitamin D levels are associated with increased MS disease activity.
After diagnosis — what’s next
Although your symptoms can be helpful for making your initial MS diagnosis, we understand that one of your biggest concerns after diagnosis is controlling symptoms so you can get back to life.
Fortunately, there are many ways to tackle MS symptoms using medicine and the latest therapies, and we’ll partner with you to fight back against those you find most bothersome.

