
Outpatient Rehabilitation
Physical therapy, occupational therapy and speech therapy
Ranked as the number one rehabilitation center in Ohio by Newsweek and as one of the ‘Best Hospitals’ for Rehabilitation by U.S. News & World Report, our team of experts at The Ohio State University Wexner Medical Center is here for you at every stage of your recovery.
Our goal is to create a personalized plan to get you back to doing what’s important to you. We specialize in a wide range of rehabilitation and therapy care, from acute services to inpatient and outpatient occupational, physical and speech therapy. The Ohio State Wexner Medical Center offers unparalleled specialized rehabilitation services for many neurological, orthopedic, balance and women’s health conditions, wheelchair seating, mobility and more.
Ohio State’s rehabilitation and therapy teams work together to provide an individualized plan that includes many types of specialists such as physiatrists, physical therapists, occupational therapists, speech language pathologists, recreational therapists, rehabilitation engineers and music therapists. We’ll combine state-of-the-art treatments with an individualized approach to care to help you get back to enjoying the things you love most.
As an accredited provider by the Commission on Accreditation of Rehabilitation Facilities, we’re focused on providing the highest levels of quality for rehabilitation care.
At the Ohio State Wexner Medical Center, we offer several specialized physical therapy and rehabilitation services to help you no matter where you are in your journey.

We’ll help you adjust and recover after the loss of a leg, foot, arm, or hand.

The Brain Injury Rehabilitation Program offered by Ohio State’s Wexner Medical Center helps patients recover from mild, moderate, or severe brain injuries.

Overcome the effects of your cancer or any associated lymph node swelling with a personalized treatment plan.

Heart and vascular therapy so you can resume your daily activities following a cardiac event.

Our team will help you recover from injuries or issues involving bones, muscles and joints.

Learn healthy ways to mitigate and deal with your chronic pain from back issues, headaches or other conditions.
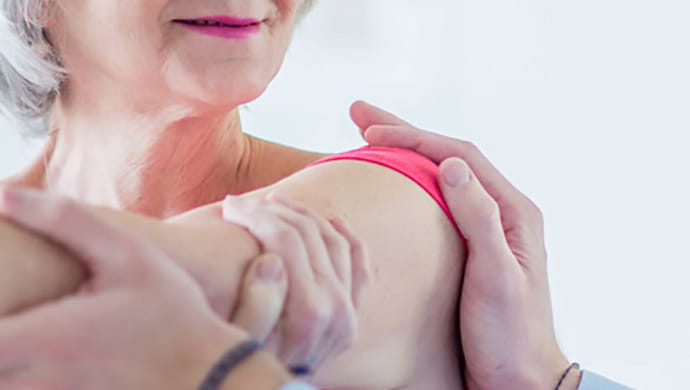
Advanced medical interventions and innovative therapies to help improve your ability to complete daily tasks.
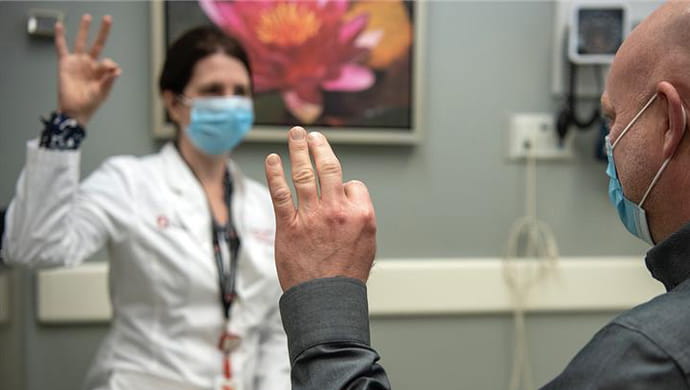
Regain your functionality, mobility and independence with our support and expert rehabilitation services.

We can help you improve your physical performance, recover from an injury and stay active for a lifetime.
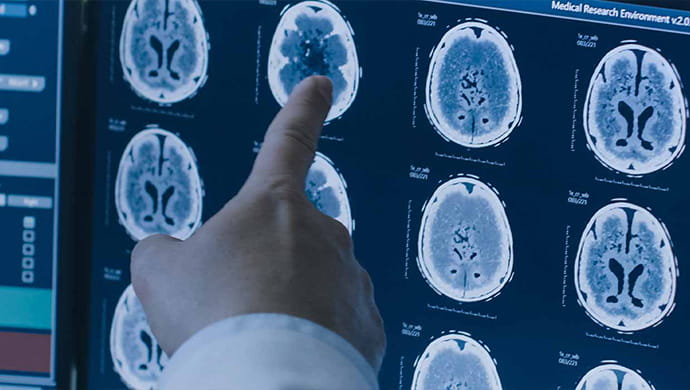
Find relief with therapy for dizziness, vertigo and other vestibular disorders and concussion.

Therapy for most pelvic floor problems.

A comprehensive list of physical therapy and rehabilitation services offered at The Ohio State University Wexner Medical Center.

Our rehabilitation services are located throughout central Ohio. For physical therapy, please contact our offices in New Albany, Gahanna or Lewis Center. Located closer to campus is the Jameson Crane Sports Medicine Institute and the Martha Morehouse Outpatient Care Center. Patients with more serious conditions may receive in-patient treatment at the Dodd Rehabilitation Hospital on the Wexner Medical Center campus. Additional locations with specialized services are available as well.
Patients with more serious conditions may receive inpatient treatment at the Dodd Rehabilitation Hospital. The facility, ranked 33rd nationally, has set the standard for inpatient care and rehabilitation for seriously injured patients. It's one of five hospitals in the U.S. chosen to participate in the NeuroRecovery Network developed by the Christopher Reeve Foundation.