Innovations at Ohio State's COPPER Laboratory
The Department of Surgery's research efforts are focused on key areas of interest that promise to yield significant results in the understanding of disease and the improvement of clinical care.

Liver Transplantation
The next step we are working on is developing a small animal (rat) model of liver transplantation to test the principals of normothermic ex-vivo liver perfusion. We will analyze animal survival, transaminases, bile production and contents, portal vein and hepatic artery pressure and flow and organ histology.Lung Perfusion
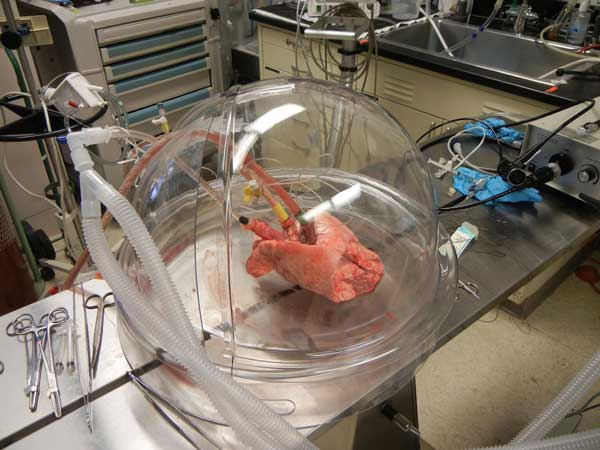 The goal of our research is to identify molecular mechanism of transplant procurement related to ischemia-reperfusion injury and develop approaches to mitigate reperfusion injury in heart and lung transplantation and cardiopulmonary bypass. The research program has evolved into its current form through integrating three scientific interests – biomedical engineering, molecular signaling and transplant medicine. The research is centered around utilizing ex-vivo lung perfusion (EVLP) to identify critical, mechanistic steps in lung injury progression. Elucidating these steps will enable a robust biologic metric to assess lung function to be defined. As a result, we will establish therapeutic approaches to mitigate acute lung injury (ALI) and subsequently recondition and protect the lung. Ultimately, the EVLP platform is ideal as a translational platform for organ resuscitation and modulation for organ transplantation.
The goal of our research is to identify molecular mechanism of transplant procurement related to ischemia-reperfusion injury and develop approaches to mitigate reperfusion injury in heart and lung transplantation and cardiopulmonary bypass. The research program has evolved into its current form through integrating three scientific interests – biomedical engineering, molecular signaling and transplant medicine. The research is centered around utilizing ex-vivo lung perfusion (EVLP) to identify critical, mechanistic steps in lung injury progression. Elucidating these steps will enable a robust biologic metric to assess lung function to be defined. As a result, we will establish therapeutic approaches to mitigate acute lung injury (ALI) and subsequently recondition and protect the lung. Ultimately, the EVLP platform is ideal as a translational platform for organ resuscitation and modulation for organ transplantation.A firm understanding of ischemia-reperfusion development and avenues to potentiate the ischemia-reperfusion injury has cross applicability to cardiopulmonary bypass, trauma, vascular surgery and other solid organ transplantation. Specifically, we have developed a cell culture based approach to identification of the mechanisms of ischemia-reperfusion injury in pulmonary artery endothelial cells and human bronchial epithelial cells.
Ex-vivo lung perfusion: small animal modelSmall animal EVLP is being developed as a platform to elucidate the mechanism identified in the cell culture approach at an organ level. The EVLP will then serve as the platform for organ modification and regeneration as these organs are then transplanted in a small animal model. Our three to five year goal is to move to clinical trials.
Liver Perfusion
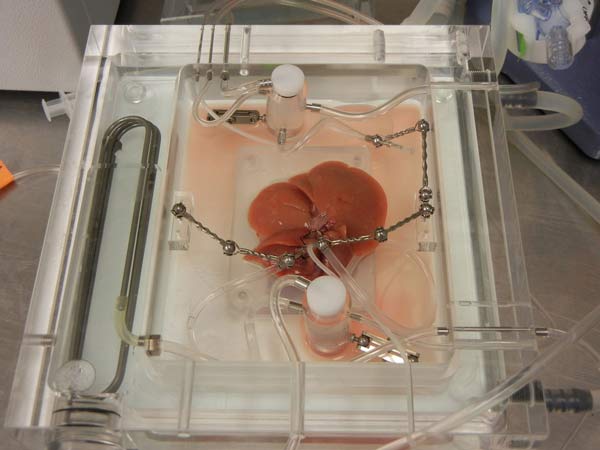
Currently, in the United States there are approximately 14,408 on the waiting list for liver transplantation with about 7,000 operations performed annually (UNOS OPTN Data 2017). The limiting factor to more widespread application of liver transplantation for the treatment of end-stage liver disease is twofold. First, there is the limited number of available donor organs for transplantation and second, is the diminished quality of those available donor organs, which leads to a decreased donor organ utilization rate and less than optimal outcomes with lower quality organs. Even modest improvements to the donor utilization rate of 10 percent could provide for many more transplants, thus expanding the donor pool significantly.
Normothermic ex-vivo liver perfusion: small and large animal modelsThe principle of normothermic ex-vivo liver perfusion that would abrogate many of the issues associated with a degredation in donor organ quality following brain death or cardiac death involves removing the donor organ from the body and supporting it on an oxygenated circuit, delivering important metabolic substrates, leaving much of the normal donor organ physiology intact. Developing a perfusate that can appropriately support a donor organ on an ex-vivo circuit will be critical to fully realizing the potential of the technology and is an important focus of the laboratory. Normothermic ex-vivo liver perfusion would therefore allow for accurate assessment of that donor organ and potentially with long enough perfusion, repair of suboptimal organs with targeted gene delivery and cellular repair molecules currently in development.
Animal models utilized in the COPPER Laboratory for normothermic ex-vivo liver perfusion:
- Rat model of normothermic ex-vivo liver perfusion using Harvard Apparatus Universal Perfusion System. Portal vein and/or hepatic artery perfusions, with the capability to measure pressure and flow, perfusate pH, pCO2, oxygen consumption, hepatic transaminases, LDH and bile production. Liver transplantation of after EVLP with full small animal microsurgical suite.
- Porcine model of normothermic ex-vivo liver perfusion using a centrifugal pump, membrane oxygenator, heater/cooler, +/- dialysis. All physiologic and metabolic parameters followed in real time, liver transplantation may be performed after perfusions. Full large animal operating room suite. Both non-survival and survival models.
Development of Acute Lung Injury Models
The lab of Dr. Samir Ghadiali investigates the neurobiology of the lung and its role in acute lung injury (ALI) and acute respiratory distress syndrome (ARDS) as a potential regenerative method in organ healing. The parasympathetic reflex pathway of the vagal nerve is vital in the homeostasis of the lung. With innovative advancements in extracorporeal membrane oxygenation (ECMO), it has become a widely available treatment option for patients with ALI/ARDS. The lab specifically study the effects of venovenous (VV) ECMO upon the lung at a molecular level targeting the role of the parasympathetic reflex pathway. Dr. Ghadiali's current work is using a swine model of ALI/ARDS in a scientific laboratory that is a fully operational surgical suite equipped with modern mechanical ventilators and ECMO circuits along with transthoracic echocardiography, bronchoscopy, fluoroscopy and near-infrared spectroscopy.The lab is also involved with a large animal brain-death model in collaboration with Dr. Bryan Whitson and Dr. Sylvester Black at The Ohio State University Wexner Medical Center. Currently, they are developing methods to improve organ preservation to improve outcomes in organ transplantation. In addition to investigating VV ECMO as potential in vivo perfusion treatment to preserve donor organs in a porcine brain-death model, they are studying the impact of brain death upon visceral organs while identifying potential targets for organ preservation and regeneration using cellular and biomedical technology.
