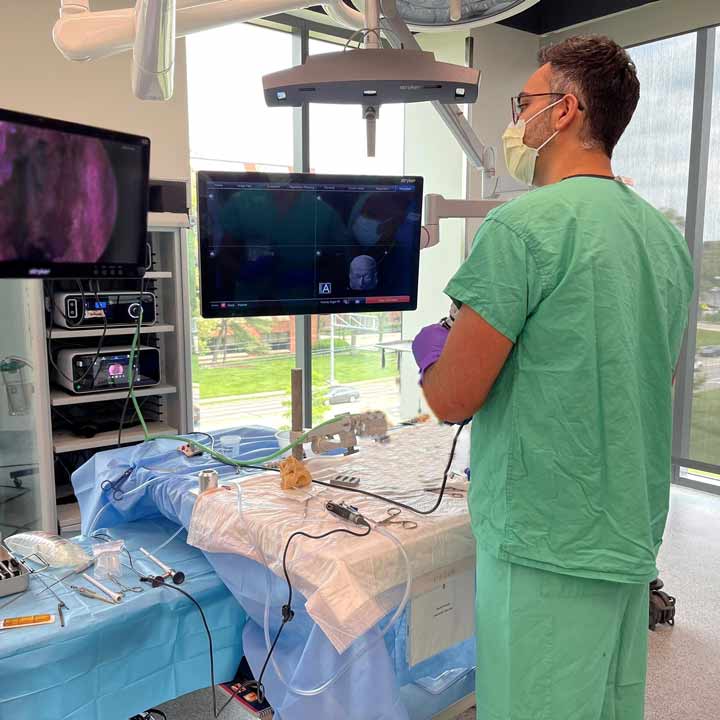
 The program offers continuing education for minimally invasive surgical techniques
The program offers continuing education for minimally invasive surgical techniques
After a two-year hiatus due to the COVID-19 pandemic, the Division of Skull Base Surgery at The Ohio State University Wexner Medical Center and The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (OSUCCC – James) brought back its hands-on endoscopic surgery course with a new format.
“We’ve been training in all types of endoscopic approaches — whatever it takes to care for the patient. That includes treating the highest complexity cases,” says Daniel Prevedello, MD, neurosurgeon and professor in the Department of Neurological Surgery at The Ohio State University College of Medicine. “There is a pioneering aspect of what we teach in endoscopic surgery, including what Ohio State brings as a multidisciplinary team. Physicians taking this course get the best experience to take back to their institutions.”
The advent of endoscopic surgery in the 1990s meant the ability to support more patients with a minimally invasive approach. Unfortunately, many of these techniques, particularly advanced endoscopic procedures, are not taught during training.
“There can be a steep learning curve for these procedures,” says Ricardo Carrau, MD, director of the Division of Skull Base Surgery at the OSUCCC – James and professor in the Ohio State Department of Otolaryngology – Head and Neck Surgery. “Many physicians never received this training in residency.”
This course aims to correct that through a hands-on approach. The first day of the course takes place at the OSUCCC – James and includes lectures and live surgery. The second and third days take place at Ohio State’s state-of-the-art Surgical Skills Lab, a venue that facilitates advanced cadaveric training.
Drs. Carrau and Prevedello have been leaders in endoscopic surgery for the treatment of skull-base and head and neck cancers over the past three decades. Dr. Carrau was among the first physicians in the world to pioneer these techniques in the 1990s and, along with Dr. Prevedello, has been teaching the course at Ohio State since 2011.
The course provides training in a controlled environment in anatomy and techniques and strategies for managing disease. Drs. Carrau and Prevedello emphasize that there are many ways of treating conditions, and these surgeries are one more tool in the toolbox.
“This course is one of many strategies to empower physicians to continue training and gain skills,” Dr. Prevedello says. “Training, like using simulators to teach an endonasal approach, is more effective and safer for complex procedures.”
To model these complexities, Kyle VanKoevering, MD, a skull-base surgeon and clinical assistant professor in the Department of Otolaryngology, developed models of difficult-to-emulate complications using 3D printing. For example, the team trained on a pediatric surgery model with a smaller cranium where the sinuses weren’t fully developed. Trainees also used models for catastrophic injury that would lead to massive bleeding — all in a controlled environment.
More than 70 physicians attend the course every year, nearly half of whom come from outside the United States In 2022, 15 countries were represented at the training.
While the course originated with endoscopic techniques, it’s evolved beyond how to do the procedure.
“We bring a comprehensive view,” Dr. Carrau says. “It’s not just surgery, but a complete strategy of how to treat patients. We try to think outside the box for how to provide more hands-on training on these aspects to participants.”
For example, some tumors were treated with surgery alone in the past, but now can be targeted with radiation therapy. The course includes a multidisciplinary approach with other specialties including anesthesiology, endocrinology, medical oncology, oculoplastic surgery, radiation oncology, radiology and reconstruction.
As the course has evolved to meet the needs of the audience, Drs. Carrau and Prevedello have fine-tuned the content to teach more advanced concepts, including moving from an anatomy-based approach to a disease-oriented one. Some topics covered in recent courses include malignancies of the sinonasal tract and meningiomas of the skull base.
“As a cancer hospital, we have a culture of multidisciplinary cooperation, including speech and physical therapy, social work, case management and others, all working in the same hallway,” Dr. Carrau says. “When it comes to cancer care, it’s important to address these aspects immediately. Through our course, we can teach others how to implement this comprehensive approach.”
The next session of the endoscopic surgery course is scheduled for May 18-20, 2023.

2025 Year in Review
See how Ohio State is shaping the field of Otolaryngology – Head and Neck Surgery.

