
First drugs ever approved for lupus nephritis
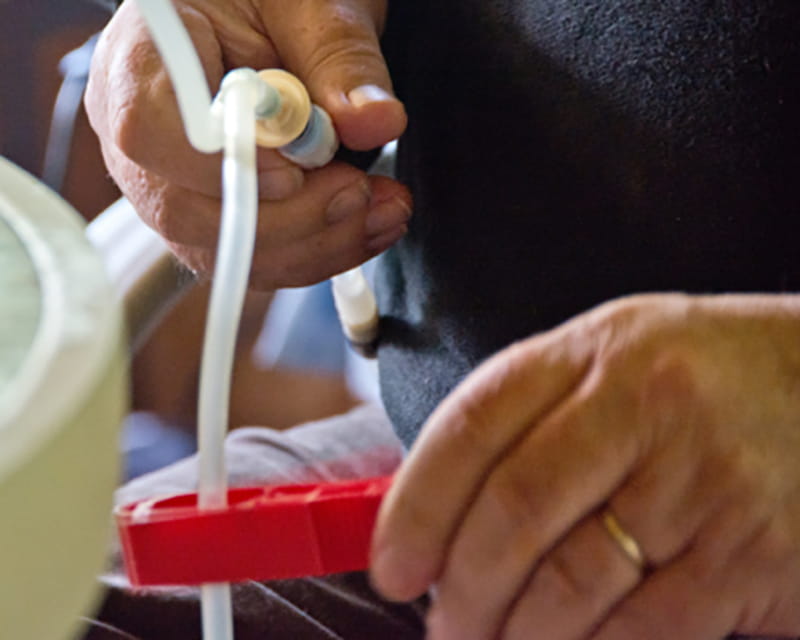 A coordinated effort by clinicians at The Ohio State University Wexner Medical Center has doubled the number of kidney disease patients receiving peritoneal dialysis.
A coordinated effort by clinicians at The Ohio State University Wexner Medical Center has doubled the number of kidney disease patients receiving peritoneal dialysis.
Their ongoing initiative, which emphasizes patient education, seeks to lower overall health care costs while improving treatment accessibility and quality of life for people who require lifesaving dialysis.
While hemodialysis and peritoneal dialysis both serve as an essential bridge to kidney transplantation, the latter option offers several advantages.
“Patients can undergo daily peritoneal dialysis treatments in the comfort of their own homes,” says Dan Spetie, MD, associate professor in Ohio State’s Division of Nephrology and director of home dialysis. “Not only does this eliminate the need for patients to travel to a hemodialysis center three times a week, but those on automated peritoneal dialysis using a cycler can undergo treatment overnight, while they sleep. This helps patients maintain more active lifestyles and possibly employment.”
In addition to offering greater flexibility, peritoneal dialysis is less expensive to deliver than in-center hemodialysis. However, only 8-10% of patients nationwide use this home-based therapy.
Dr. Spetie, who is an associate professor – clinical at the College of Medicine, says that historically, peritoneal dialysis utilization at Ohio State mirrored that in the rest of the country. But about two years ago, he and his colleagues — including nephrologists Anil Agarwal, MD, a professor – clinical at the College of Medicine, and Khaled Boubes, MD, an assistant professor – clinical at the College of Medicine — decided it was time to expand those numbers.
“Research suggests patients may not be fully aware of their dialysis options, or they’re frightened by the idea of performing their own treatments,” Dr. Spetie says. “We initiated a patient education and engagement plan to help make sure people understand the different types of dialysis available to them, including the pros and cons of each. And, as always, prior to any patient starting home dialysis, we alleviate their fears with thorough training.”
Their team of nephrologists, dialysis nurses and other clinicians focuses on two groups of patients:
They also continue to educate and encourage patients who have not yet started dialysis — but whose chronic kidney disease is progressing to end-stage renal disease — to consider home dialysis modalities, including peritoneal dialysis.
“Within the field, the standard approach to treating people who need emergent dialysis is to start them on hemodialysis,” Dr. Spetie says. “At Ohio State, we connect with these patients at the bedside to let them know they have a choice in their dialysis treatment. We can insert their catheter and begin peritoneal dialysis treatment and training before they leave the hospital. This means patients don’t have to start one type of dialysis and eventually switch to another, which would require them to have two different vascular access procedures.”
Today, 32 Ohio State patients are on peritoneal dialysis — a two-fold increase compared to just 18 months ago.
Ohio State’s efforts are timely, especially considering the July 2019 passage of the Advancing American Kidney Health initiative. Launched by the U.S. Department of Health and Human Services (HHS), it aims to improve the lives of Americans suffering from kidney disease, expand treatment options and reduce costs.
“Our own expansion dovetails nicely with the HHS initiative,” Dr. Spetie says. “One of their national goals is to make it easier for patients to receive dialysis at home.”
Through the initiative, the Centers for Medicare & Medicaid Services (CMS) has reviewed potential refinements to the End-Stage Renal Disease (ESRD) Prospective Payment System to facilitate Medicare beneficiaries’ access to certain innovative treatment options. To that end, CMS is providing financial incentives to help clinicians better manage care aligned with beneficiaries’ preferences regarding home dialysis.
Dr. Spetie says he and his colleagues will continue making sure their kidney disease patients are aware of their dialysis options, so they can make informed decisions about their treatment.
“Our expansion is too recent to establish any outcomes data,” he adds. “However, as we transition more patients to peritoneal dialysis, we intend to track and compare outcomes that should contribute more evidence confirming the safety and efficacy of home therapies.”