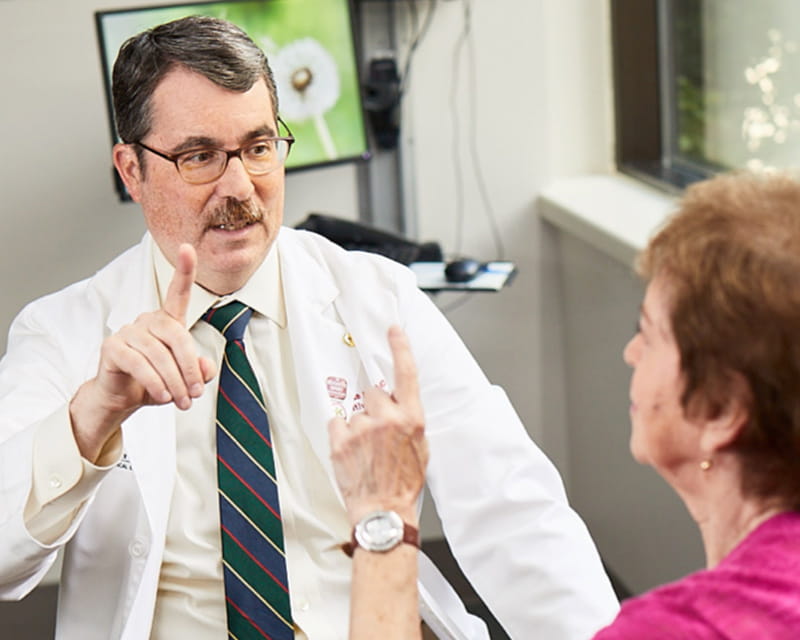
Ohio State researchers identify new biomarkers that differentiate Lewy body dementia from Alzheimer’s and Parkinson’s
 Ohio State University Wexner Medical Center uses innovative technique to reprogram cells and reverse neurological deficiencies
Ohio State University Wexner Medical Center uses innovative technique to reprogram cells and reverse neurological deficiencies A novel method of gene therapy that shows success in reversing neurological deficiencies from a rare childhood genetic disorder also holds promise for common neurodegenerative diseases, such as Parkinson’s and Alzheimer’s diseases.
Developed by researchers at The Ohio State University Wexner Medical Center, The Ohio State University College of Medicine and the University of California San Francisco, the genetic therapy treatment reprograms cells to produce chemicals needed for the brain to properly function.
During surgery, doctors infuse a benign virus programmed with specific DNA into precisely targeted areas of the brain. The virus introduces a new operating code to the targeted cells, says Krystof Bankiewicz, MD, PhD, principal investigator and a professor of neurological surgery at the Ohio State Wexner Medical Center.
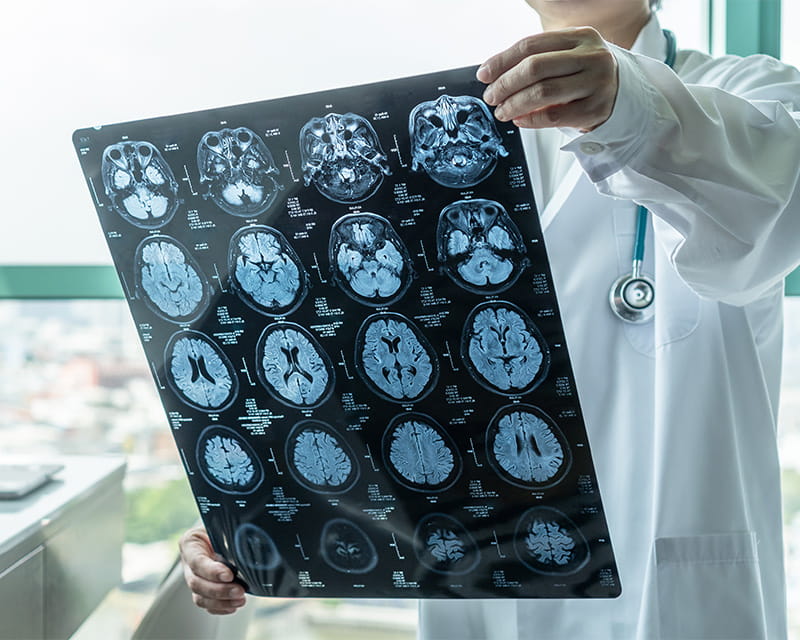
During surgery, neurosurgeons infuse coded virus cells directly into the brain. The infusion occurs slowly as doctors monitor exactly how it spreads within the brain using real-time MRI.
The patient undergoes continuous MRI imaging during the procedure, as the surgical team watches what’s happening in the brain to ensure the infusion reaches the targeted brain tissue. Clinical trials are underway to test this procedure in patients living with debilitating and incurable neurological conditions.
Children born with AADC (aromatic L-amino acid decarboxylase) deficiency are missing an enzyme that produces dopamine in the central nervous system.
Only about 135 children worldwide are known to have AADC deficiency, which causes severe physical and developmental disabilities. These children lack muscle control and usually can’t speak, feed themselves or hold up their heads. They also suffer from seizure-like episodes called oculogyric crises that can last for hours.
When children with AADC receive this gene therapy, they show amazing results.
“Remarkably, these episodes are the first symptom to disappear after gene therapy surgery and they never return,” says Dr. Bankiewicz, who co-authored a July 2021 study published in Nature Communications.
“In the months that follow, many patients experience life-changing improvements,” he says. “Not only do they begin laughing and have improved mood, but many are able to begin speaking and even walking. They are making up for the time they lost during their abnormal development.”
In a National Institutes of Health-funded clinical trial with seven children:
The Ohio State gene therapy team also is testing this method with Parkinson’s disease patients. They performed the first-ever gene therapy brain infusion in a Parkinson’s patient in September 2020.
The treatment uses a viral vector to deliver a naturally occurring growth factor called glia cell derived neurotrophic factor (GDNF) to the putamen, a deep brain structure affected by Parkinson’s disease.
There is ample evidence that GDNF has promise as a therapy for Parkinson's disease, as shown in animal and cell culture models. Until now, there was no way to deliver treatment deep into the brain.
“I’ve been investigating therapeutic gene therapy approaches for Parkinson’s disease for nearly 30 years, and this marks a significant milestone that may lead to major therapeutic opportunities,” says Dr. Bankiewicz, who founded the biotech startup Brain Neurotherapy Bio Inc. in 2018 to develop gene therapies for neurological disorders.
Bankiewicz and his team hope the Parkinson’s gene therapy surgery — a one-time treatment — provides ongoing benefits to slow disease progression.
The safety and effectiveness of gene therapy for AADC deficiency will get even more study thanks to a $14.6 million award from The National Institute of Neurological Disorders and Stroke in September 2021.
The grant will fund a new multi-center clinical trial with patients at The Ohio State University and at the University of California San Francisco.
The research will build on Dr. Bankiewicz’s earlier clinical trial and an additional study of 15 children under an ethics committee-approved compassionate use program in Poland, he says.
The ability to deliver a functional copy of a missing gene provides hope to many.
“This will pave the way for the registration of future gene therapies to treat other neurological disorders,” Dr. Bankiewicz says.

Ohio State researchers identify new biomarkers that differentiate Lewy body dementia from Alzheimer’s and Parkinson’s

Biomarker breakthroughs at Ohio State transform disease diagnosis, predictability and treatment
The Ohio State University Wexner Medical Center pushes boundaries for neurological care