
Innovation and Research
 In a perfect world, patients with head and neck squamous cell carcinoma who need curative surgery would get the surgery within days or weeks of their diagnosis. Unfortunately, that’s not always the case, since issues related to surgical planning, preoperative clearance and scheduling—not to mention pandemics—can create delays. Such delays can cause anxiety in patients, but what impact do they have on survival rates? Researchers at The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (OSUCCC – James) recently explored this question and found that a delay of 67 days or more after initial diagnosis independently resulted in worse survival. Their study, published in the Annals of Surgical Oncology, is the first to correlate surgical delays and head and neck cancer survival rates.
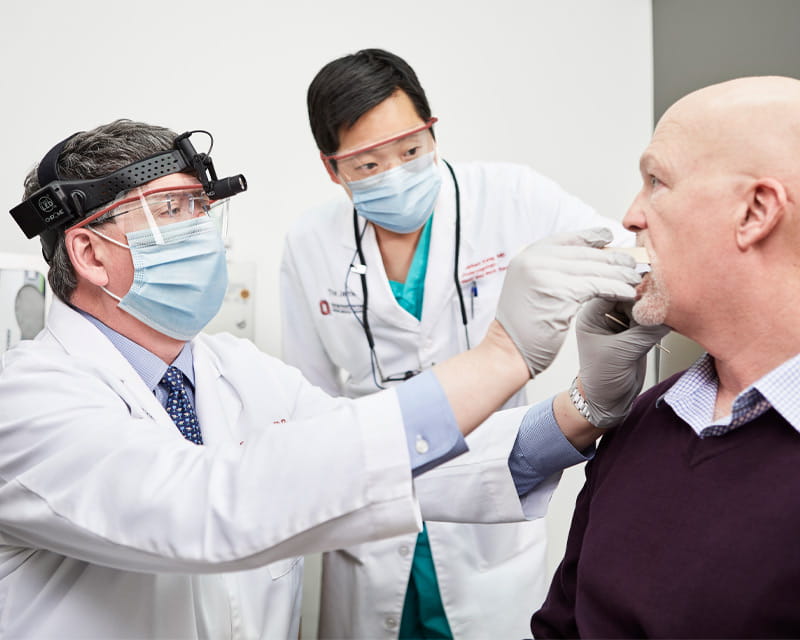
In a perfect world, patients with head and neck squamous cell carcinoma who need curative surgery would get the surgery within days or weeks of their diagnosis. Unfortunately, that’s not always the case, since issues related to surgical planning, preoperative clearance and scheduling—not to mention pandemics—can create delays. Such delays can cause anxiety in patients, but what impact do they have on survival rates? Researchers at The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (OSUCCC – James) recently explored this question and found that a delay of 67 days or more after initial diagnosis independently resulted in worse survival. Their study, published in the Annals of Surgical Oncology, is the first to correlate surgical delays and head and neck cancer survival rates.
“Everyone knows intuitively that surgical delays are harmful. Our study shows that they are actually more harmful than we thought,” says Stephen Kang, MD, a head and neck cancer surgeon at the OSUCCC – James and the study’s co-principal investigator. “Our analysis isolated the effect of treatment delay on survival by controlling for stage, tumor size and progression, tumor site, positive margins, patient age and medical comorbidities. Even controlling for all of those factors, we found that surgical delays impacted survival. We hypothesize that when surgery is delayed, there is ongoing subclinical tumor spread and progression that can’t be captured on diagnostics but ultimately causes death. That’s the real impact of waiting.”
The retrospective cohort study included 37,730 patients in the National Cancer Database with head and neck squamous cell carcinoma who underwent primary surgical management from 2004 to 2016. Biostatisticians Guy Brock, PhD, and Songzhu Zhao, MS, from The Ohio State University College of Medicine’s Department of Biomedical Informatics and Center for Biostatistics worked with Dr. Kang and other researchers on the team to analyze the data. They used a statistical method called cubic spline analysis that allowed them to determine the association between time to surgery and survival without assuming a linear relationship.
Among the study’s findings:
“Many things are completely out of the medical team’s control when caring for patients with head and neck cancer, but time to surgery is something we can immediately modify,” Dr. Kang says. “How surgeons counsel patients about timing, triage surgery schedules and optimize preoperative clearance can all contribute to minimizing delays and improving survival.”
First author Chandler Rygalski adds that the study has implications for triaging surgical patients in the COVID-19 era. “We started planning this study in 2018 and were in the midst of writing it when COVID-19 forced the suspension of elective surgeries at the medical center,” says Rygalski, a third-year medical school student who is planning to specialize in head and neck surgery. “If health care systems face similar suspensions in the future, this paper provides evidence that patients with head and neck cancer should be among those prioritized for surgery.”

Innovation and Research

Vestibular Innovation

Leading the Way