 As we’ve learned in 2020, a global health pandemic can change the best laid plans—including those for medical education.
As we’ve learned in 2020, a global health pandemic can change the best laid plans—including those for medical education.
Early in the COVID-19 crisis, medical schools nationwide paused students’ clinical rotations to help reduce spread of the novel coronavirus and to conserve personal protective equipment.
The move was necessary at the time, but for Michael Wells, MD, medical student clerkship director in the Department of Ophthalmology and Visual Sciences at The Ohio State University Wexner Medical Center, it was also concerning.
Already troubled by medical students’ dwindling exposure to ophthalmology as a specialty nationwide, Dr. Wells knew that suspending rotations would only compound the problem. And since clinical experiences are what typically lead students to pursue an ophthalmology career, the situation was doubly worrisome.
“The ophthalmology residency match is an early match, too, compared to all the other specialties,” he says. “Students really need to get exposure early on to decide if they want to try to go into ophthalmology.”
A virtual approach, a quality experience
Determined not to lose students interested in ophthalmology, Dr. Wells set out to create a clinic experience that would be beneficial for students, as well as safe for students and patients alike during the coronavirus outbreak.
What resulted was a four-week virtual rotation that essentially combines telehealth technology with tele-education. Described in detail in the Journal of Academic Ophthalmology, the rotation is available to fourth-year med students. It provides a shadowing experience that mimics every aspect of the experience students would normally have in person.
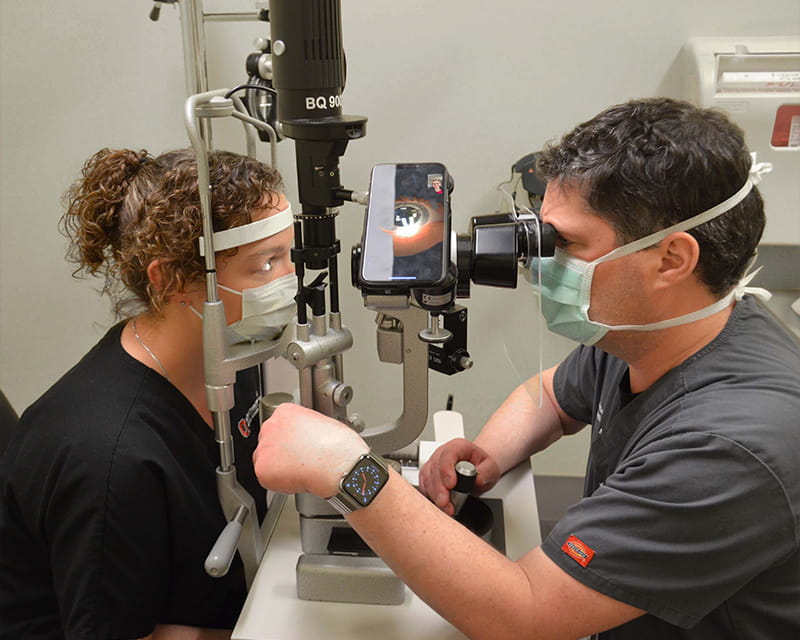
Videoconferencing apps, iPhones and special equipment that allow students to take part in slit lamp exams while offsite make the experience possible. During patient appointments, the iPhone is carried from room to room and placed in a manner that allows the student to observe the entire visit remotely. This includes:
- The patient workup with ophthalmic technicians and imaging specialists
- Patient interviews and procedures performed by the attending ophthalmologist
- Virtual slit lamp exams piloted at the Ohio State Havener Eye Institute and the UCLA Stein Eye Institute
Students also participate in weekly half-day didactics in which they review ophthalmology cases virtually.
According to Dr. Wells, the slit lamp exams are what set apart the experience at the Ohio State Wexner Medical Center. Using special adapters, the onsite team can place the iPhone in the slit lamp’s viewing lens, allowing students to directly participate in the patient examination. “They can see what we’re seeing and hear what we’re hearing,” he says.
“Other programs have been doing didactics, lectures, quizzes and other types of online learning,” Dr. Wells adds. “They’ve also included telehealth visits, where the student is basically doing the history and maybe a little bit of a physical examination. Our program is unique in that we are actually allowing students to see things with the slit lamp that the attending physician is able to see as well. It’s a bit more in-depth and more detailed.”
From challenges come opportunities
The first virtual rotations occurred in April and May and were very well received. “The students have been incredibly positive,” Dr. Wells says. “We’ve gotten really, really good feedback.”
So far, a handful of students have participated, but numbers are projected to increase next year. The virtual rotation is expected to be an important offering throughout the pandemic and beyond.
“I think it has a lot of potential applications,” Dr. Wells says. “Some students from other institutions can’t afford the expense of doing away rotations, and this year, the (Association of University Professors of Ophthalmology) recommended against all away rotations due to the pandemic.”
A virtual rotation provides the experience without the travel. “This will allow students to become familiar with the Ohio State Wexner Medical Center and our residency program even after the COVID-19 pandemic is done,” he says.
Dr. Wells also sees potential for virtual slit lamp exams in telehealth and teleconsultations. When an ophthalmologist needs a colleague’s opinion or assistance, the technology makes it possible to conduct an exam from a remote location. “The clinical implications in the future are going to be pretty broad.”
While COVID-19 has presented plenty of challenges, it’s worth noting that good can come out of bad. “Education and health care don’t stop because of a pandemic,” Dr. Wells says. “Innovation can sometimes come about because of a crisis like this.”

