Comprehensive Esophageal Health Center opens with more convenient, streamlined care
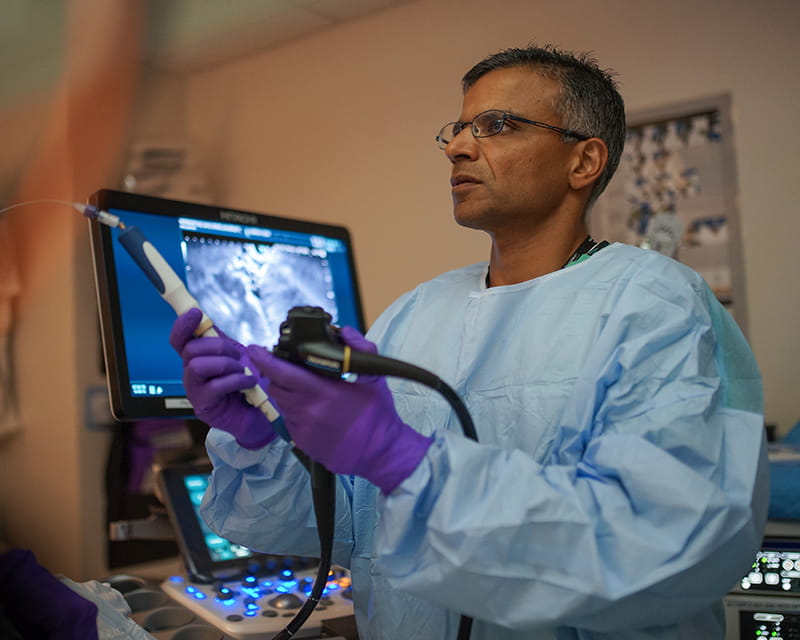
Pancreatic cancer continues to have a high mortality rate, and long-term survival has not improved as it has in many other cancers. This is largely because pancreatic cancer is most commonly diagnosed when already in an advanced stage or when it has metastasized to other parts of the body.
Pancreatic cystic lesions can be either benign or precancerous, and they are increasingly diagnosed, primarily due to improved detection during imaging studies. Accurate diagnosis and resection of premalignant pancreatic lesions and avoiding unnecessary surgery of otherwise benign cysts is critical, as it will influence future prognosis and treatment plans. However, there are limited ways to accurately identify precancerous or malignant pancreatic cystic lesions. Current methods for diagnosing pancreatic cysts, such as MRI or CT scan, endoscopy ultrasound (EUS) and diagnostic fluid aspiration from pancreatic cysts, often yield suboptimal or indeterminate results.
A prospective study conducted at The Ohio State University Wexner Medical Center and recently published in the journal Clinical Gastroenterology and Hepatology provides evidence of a procedure with distinctly increased diagnostic accuracy. Compared to the existing standard of care (diagnostic accuracy around 70%), Somashekar Krishna, MD, MPH, a gastroenterologist in the Division of Gastroenterology, Hepatology and Nutrition, and his team have achieved a 96% accuracy rate using EUS-guided, needle-based confocal laser endomicroscopy to detect precancerous mucinous pancreatic cystic lesions. Mucinous lesions are at a higher risk for harboring or turning into invasive pancreatic cancer compared to non-mucinous cysts. This finding provides a more definitive way to diagnose precancerous or cancerous pancreatic cysts, and will also help prevent unnecessary surgical procedures for patients with benign lesions.
Dr. Krishna’s team has performed the highest number of laser endomicroscopy procedures in the United States for pancreatic cysts and was also the first to validate diagnostic endomicroscopy patterns among independent external collaborators and combine DNA-markers from the cyst fluid with endomicroscopy images to optimize diagnosis. More recently, using endomicroscopy images, the research team has demonstrated the application of computer-aided diagnosis and machine learning in automated risk stratification of mucinous pancreatic cysts. Dr. Krishna is also leading a multicenter study involving more than 10 academic institutions in the U.S. to replicate the results achieved at the Ohio State Wexner Medical Center.
Due to the limitations imposed by existing diagnostic strategies leading to misdiagnosis of malignant pancreatic cysts or unnecessary pancreatic surgeries, minimally invasive procedures such as EUS-guided endomicroscopy are powerful adjuncts to the current multimodality approach in managing patients with pancreatic cysts. Patients with pancreatic cysts can hope for fewer invasive procedures, more accurate diagnosis and risk assessment, and appropriate early surgical intervention.