Comprehensive Esophageal Health Center opens with more convenient, streamlined care
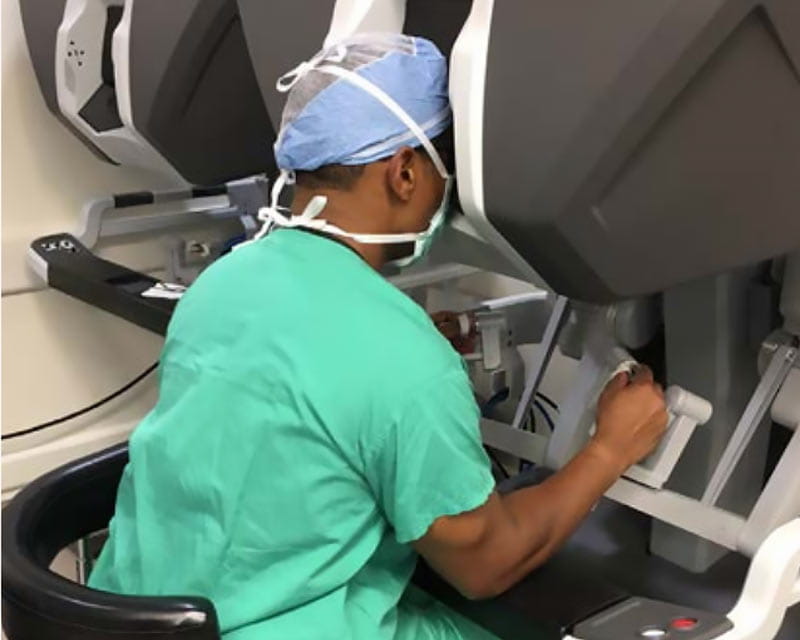 Robotic-assisted surgeries benefit patients, surgeons; expand research and training opportunities
Robotic-assisted surgeries benefit patients, surgeons; expand research and training opportunitiesGeneral and gastrointestinal surgery experts Vimal Narula, MD, and Bradley Needleman, MD, at The Ohio State University Wexner Medical Center are expanding their extensive base of robotic surgery experience by building a vibrant subspeciality in robotic metabolic and bariatric surgery.
The team of internationally known surgeons now performs the robotic loop duodenal switch procedures, adding the technique to Ohio State’s bariatric surgery program.
“We use robotics for other general surgery operations and saw benefits for it in bariatrics,” Needleman says.
Narula and Needleman have performed thousands of gastric bypasses laparoscopically, so converting to a robotic procedure was a decision they made to see if they could improve outcomes and help reduce pain, shorten hospital stays and minimize complications for patients.
As the two surgeons became comfortable with the da Vinci DXI robotic instrumentation for bariatric procedures, they saw not only potential benefits for patients but for training new and practicing surgeons.
Narula and Needleman began providing robotic bariatric surgery before the COVID-19 pandemic, but volumes dropped once the new limitations on elective surgery took hold. The team is thrilled to be ramping up again.
Robotics is not new to Ohio State’s surgeons. The DaVinci systems have been at Ohio State for more than 20 years, and surgeons have not yet reached the potential of what the approach can offer patients, Needleman says. Specialties at Ohio State who are utilizing the latest robotic technologies include cardiac surgery, general surgery, gynecology, otolaryngology, thoracic surgery, urology and even breast surgery.
The potential for growth in this area is huge. A robotic operation requires less assistance, as the surgeon is able to use four operating arms at the same time, Needleman says.
To do that laparoscopically requires a skilled assistant surgeon. Robotics eliminates the need for a second expert assistant and opens the door for advanced practice providers to assist at the bedside with instrument exchanges, passing suture and retraction.
The loop duodenal switch is a newer procedure like a sleeve gastrectomy that also includes bypassing a significant portion of the small bowel.
This loop duodenal switch provides more weight loss than a sleeve gastrectomy, without significant risk of nutritional deficits. The procedure may also have fewer complications than a gastric bypass, including marginal ulcers.
The loop duodenal switch can be used as a:
“Once patients with very high BMIs lose weight, we can then more safely perform the more challenging part of the operation,” Narula says.
Robotic bariatric surgery provides multiple advantages.
Obese patients present with thick abdominal walls that require lots of strength from the surgeon to maneuver instruments.
For surgeons, robotic systems:
For patients, robotic bariatric surgery provides:
As Narula and Needleman learned robotic techniques for bariatric procedures, applying them to teaching standards was top of mind. It is predicted that in the next few years, 1 in 4 of all bariatric surgeries in the United States will be performed robotically, Needleman says.
The advanced minimally invasive surgeons at Ohio State train fellows in a variety of surgical techniques, so new surgeons are prepared to provide the best care to patients no matter what practice they join, Needleman says. Often the surgical preferences of a practice dictate which procedures an individual surgeon is most likely to adopt and perform.
“We don’t want the fellows only knowing one way to do these procedures,” Narula says. “It’s important for the next generation of surgeons to know all the different techniques including laparoscopic and robotic. Robotics may open up more job opportunities for fellows once they complete their program.”
Research plays a key role in the bariatric surgery program’s expansion into robotic techniques. At the Ohio State Wexner Medical Center, surgeons are performing the loop duodenal switch under an institutional review board (IRB) authorization.
The team is collecting data from all patients who receive the procedure as a primary or secondary treatment. Narula says they want to understand how patients respond to determine the short- and long-term effects of the procedure.
The surgeons at the Ohio State Wexner Medical Center also are studying robotics to find the best ways to train new surgeons.
They can harness data from the surgical device and its computer to get information on the efficiency of the operations, as well as individual data on a specific surgeon’s movements and technique.
A dual console robotic surgery system lets an experienced surgeon and a fellow work side by side while tracking each surgeon’s movements with data and video. This provides objective feedback and builds a database of how to use robotics to deliver better, faster and safer procedures.
“We can use that to give surgeons feedback on different points of the operation to help them improve,” Narula says.
As the data collection continues, intuitive robotic training programs will follow.
“Eventually we have the goal of being a national training powerhouse for robotic bariatric surgery,” Needleman says.