How do COVID-19 tests differ?
Editor’s note: As what we know about COVID-19 evolves, so could the information contained in this story. Find our most recent COVID-19 blog posts here, and learn the latest in COVID-19 prevention at the Centers for Disease Control and Prevention.
Ohio Gov. Mike DeWine’s recent positive test for COVID-19 created some confusion, primarily because follow-up test results were negative, showing that he wasn’t infected with the virus.
How did the governor receive what we in the medical community refer to as a “false positive?” To understand how this happened, we have to look at the difference between the two types of tests that were administered to the governor. The first test Gov. DeWine received was an antigen test conducted in Cleveland, prior to a scheduled meeting with President Trump. The follow-up testing was performed using a PCR test.
I like to think of the difference between these two tests as similar to the difference between a powerful telescope versus binoculars. The telescope can provide a close-up look at a distant star, while the binoculars offer a slightly enhanced view of the full night sky.
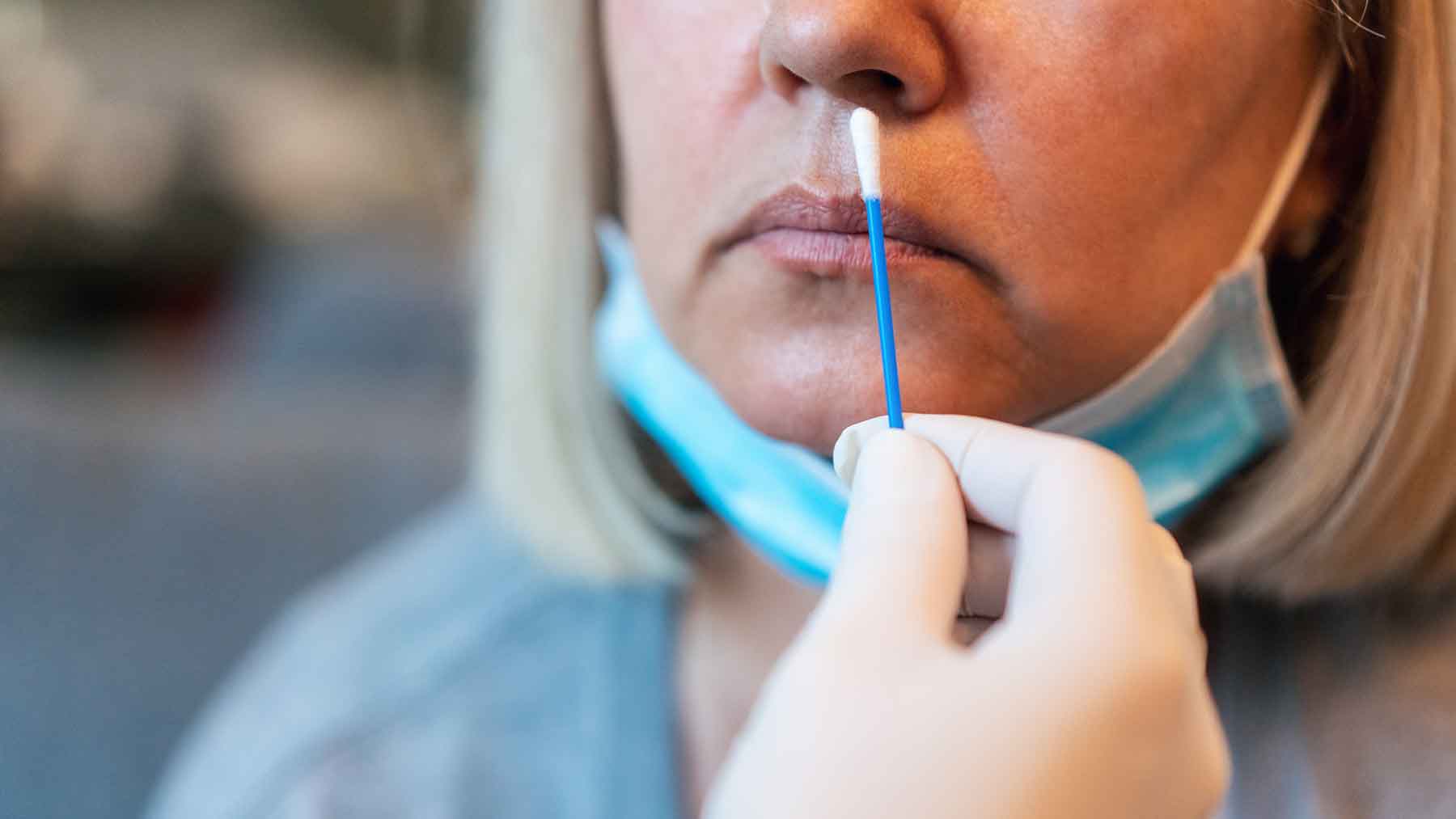
An antigen test looks for particular proteins that exist on the surface of the virus. Like the binoculars that might miss a few stars, the antigen test can’t see all of the details. But the results of this test can be read quickly, usually within minutes. Antigen tests exist for diseases like strep throat and are used when rapid results are the most important goal.
A PCR test provides the additional details that a powerful telescope would offer. PCR stands for polymerase chain reaction. With this process, a small amount of genetic material such as RNA is amplified. PCR can detect very small amounts of virus and the tests are incredibly specific for COVID-19 versus other coronavirus, but because it requires both specialized equipment and highly-trained laboratory professionals to monitor the process, it is slower and more expensive.
The rapid antigen test can be a valuable tool in our efforts to contain the spread of the coronavirus. It can be administered quickly, at the point of care such as a doctor’s office. Rapid results offer the opportunity for immediate isolation of patients infected with COVID-19. Along with isolation, patients and medical professionals can start contact tracing. This means that friends and relatives who have had recent contact with the patient can be told of their potential risk of exposure and possible infection. Those friends and relatives can then take precautions to avoid infecting others.
More than 1.6 million tests for COVID-19 conducted in Ohio have been run with the PCR method. As we learn more about the coronavirus, the antigen tests will become more accurate. In the meantime, an occasional false positive may cause confusion, but will still provide us with important information to help us stop the spread of this new, highly infectious virus.
In summary, both tests are important tools in our fight against disease, but it is important to understand the role – as well as the strengths and weaknesses of each.
Peter Mohler is the chief scientific officer for The Ohio State University Wexner Medical Center, vice dean for research at the Ohio State College of Medicine and director of the Dorothy M. Davis Heart & Lung Research Institute.




