
Sen. Brown tours COVID-19 testing site at CAS
Sen. Brown talks with members of the Ohio National Guard who’ve joined health care workers across the state on the front lines in the battle against COVID-19.
Editor’s note: As what we know about COVID-19 evolves, so could the information in this story. Find our most recent COVID-19 blog posts here, and learn the latest in COVID-19 prevention at the Centers for Disease Control and Prevention.
There’s a lot of talk about COVID-19 antibodies — how we develop them, how long they last and what they can do to protect us from severe symptoms of COVID-19. We’re here to break down the answers to these questions on behalf of The Ohio State University Wexner Medical Center’s Center to STOP-COVID (Serological Testing to Improve Outcomes from COVID-19), an interdisciplinary research effort to study the long-term effects of COVID-19.
What are antibodies?
Antibodies are specialized proteins that are part of your immune system. They help protect against viruses, bacteria and other foreign substances.
In the case of COVID-19, after you’re infected with the SARS-CoV-2 virus, your immune system recognizes the virus as a foreign substance and forms antibodies against it. These antibodies provide some level of protection against future infections because they will recognize the virus as a danger and trigger your immune system to attack it.
How does the COVID-19 vaccine help produce antibodies?
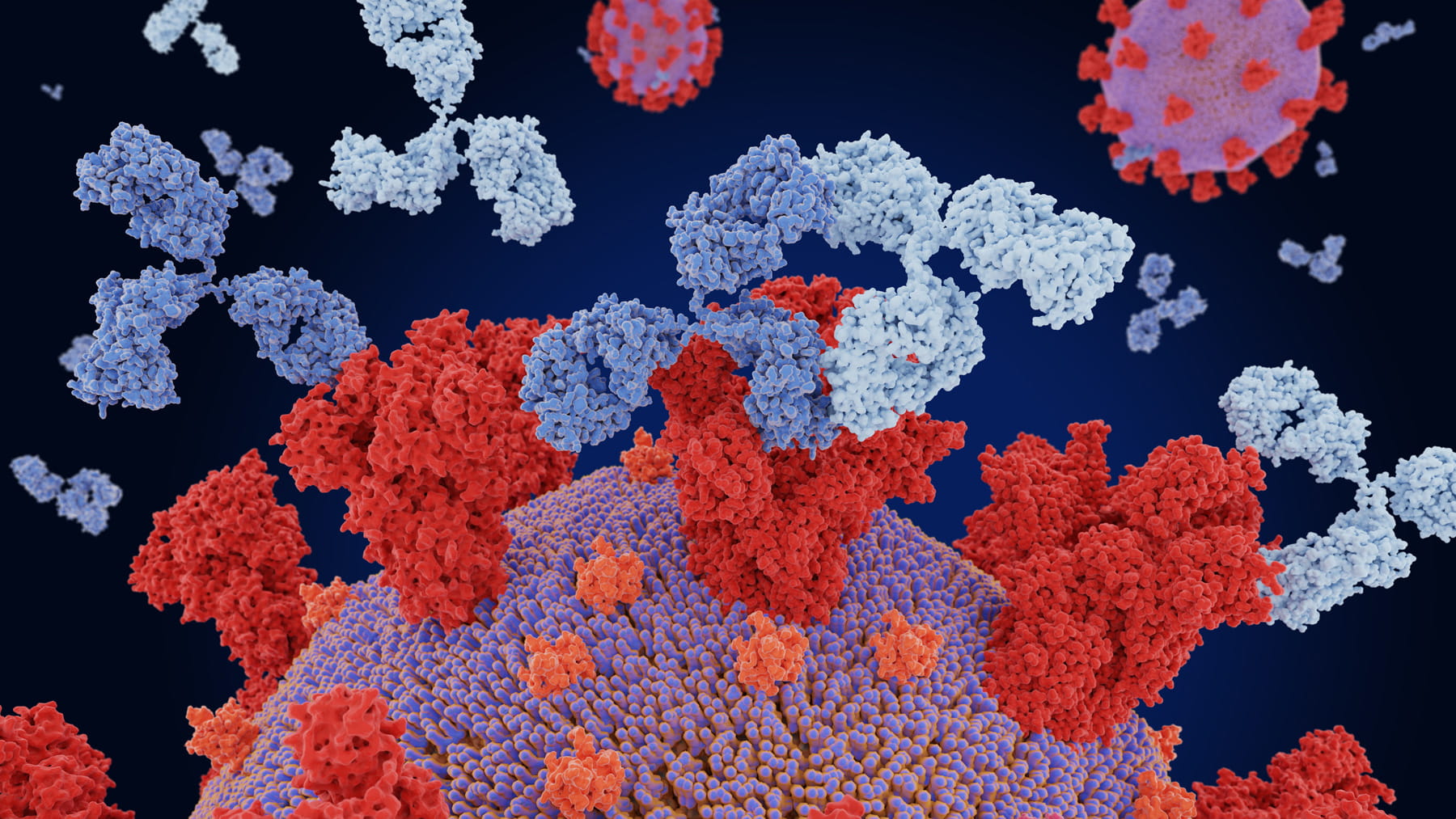
COVID-19 vaccines work by exposing your immune system to an antigen that resembles a piece of the spike protein found on the surface of the virus that causes COVID-19. The antigen stimulates your immune cells to develop antibodies against the spike protein.
If you’re exposed to the virus that causes COVID-19 later on, your immune cells recognize the spike protein as a foreign invader and trigger your immune system to attack the virus. This typically results in either no infection at all or a “breakthrough” infection. Breakthrough infections are infections in patients who have been vaccinated, and they tend to result in much milder symptoms than you would have had without the vaccine.
Can everyone develop antibodies?
People with weakened immune systems have lower ability to develop a strong immune response after vaccination. That’s why people who fall into this group, as well as others with certain medical conditions, may be eligible to receive a third dose of the Pfizer or Moderna vaccines. You should consult with your primary care provider to decide what’s best for you.
Can I be tested to determine my antibody level? What level is considered ‘positive’?
There are several types of tests available that can determine if you have antibodies to SARS-CoV-2. You may hear this referred to as serology testing. A positive antibody test may indicate that you have had a COVID-19 infection or that you have been vaccinated against COVID-19.
Antibody testing isn’t recommended to diagnose COVID-19, monitor response to vaccination, or to determine the need for vaccination in an unvaccinated person.
Antibody testing is used to determine if a person has had an infection with SARS-CoV-2 in the past. It might be recommended for public health use or if someone without a documented history of COVID-19 is showing possible complications from COVID-19, to confirm whether they did actually become infected at some point.
Because of the ways different types of antibody tests are run, we don’t look at a specific number or level to determine if a person might have an adequate level of protection. But we can determine if a person has antibodies or not, and depending on the type of test, we may be able to determine if the antibody level is low or high.
More info: