Facial plastic surgeon restores paralyzed smiles
We all know the power of a smile. Research demonstrates that smiling is the most powerful facial expression. It conveys happiness, stimulates positivity and has been shown to reduce stress.
That’s why it can be heartbreaking to those who lose their ability to smile through facial paralysis. They might have Bell’s palsy, the most common cause of a lost smile. Other causes include trauma, injury occurring during surgery, stroke, parotid (salivary gland) cancer, or vestibular schwannoma, a noncancerous tumor in the inner ear. Then, there are congenital causes such as Moebius syndrome, a rare neurological condition.
What’s in a smile?
Smiling is complex. On average, it can take 12 muscles or more for a person to smile, and every person smiles differently. This makes restoring a smile very complicated.
There are three basic types of smiles, as described by Leonard Rubin in 1974:
- The “Mona Lisa” smile – where the corners of the mouth go up and outward and upper teeth are exposed. The dominant muscle action is from the zygomaticus major muscles. This type of smiling is most common.
- The “canine” smile – where the canine teeth and upper gums are exposed. The dominant muscle action is from the levator labii superioris muscles.
- The “full dentured” smile – where the lips are pulled back strongly, showing both upper and lower rows of teeth. All muscles are dominant.
Smiles also are sometimes described as “Duchenne” smiles, which demonstrate both zygomaticus major muscle contraction as well as eye muscle contraction, causing cheeks to raise high. The addition of this eye wrinkling has been used to differentiate “genuine” versus superficial or “say cheese” smiles.
Restoring a lost smile
When the facial nerve is disrupted, the facial muscles lose their nerve supply, or become denervated. Depending on where the facial nerve is affected, all or some of the facial muscles may be involved. After about two years of denervation, facial muscles undergo irreversible atrophy and fibrosis.
Without innervation to the facial muscles, the face loses symmetry and movement. With a lower facial paralysis, the paralyzed side of the face droops and the normal side appears to be relatively hyperanimated. The central lip might pull toward the normal side, creating a highly asymmetric smile that almost appears to look like a snarl.
The options for smile restoration largely depend on the cause, type (complete versus incomplete), and duration of facial paralysis. Because the duration of facial paralysis is critical to what interventions can be offered, I recommend that patients seek out a facial nerve specialist if they aren’t experiencing improvement within three to six months of developing acute facial paralysis, regardless of cause.
Treatment options
Nerve transfers
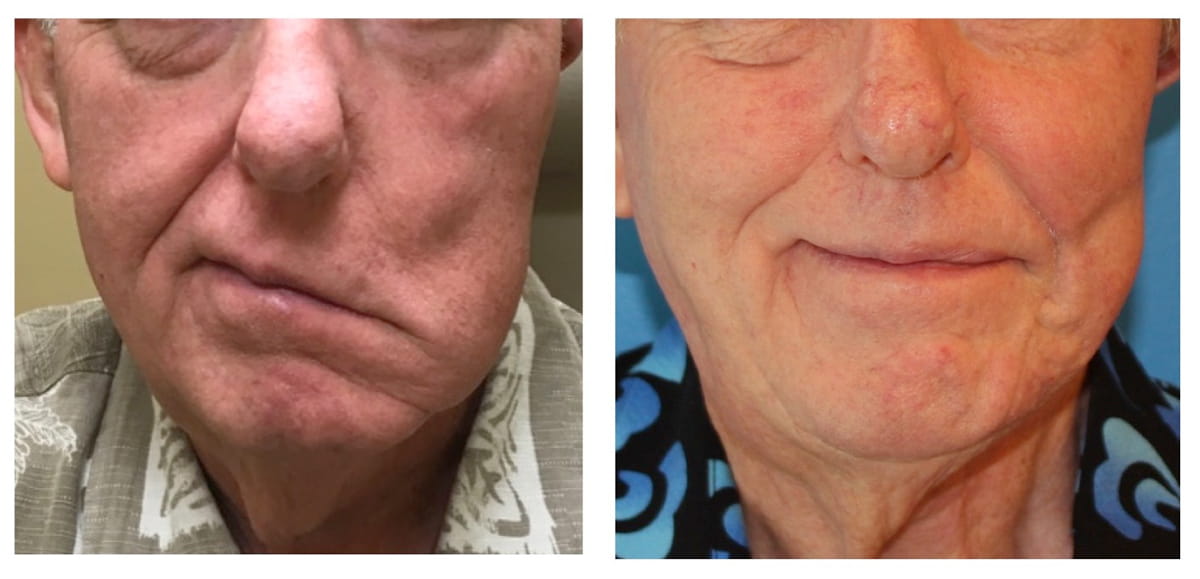
While a number of nerves can be used in this procedure, the masseteric nerve transfer is most common. It’s a nerve that moves the masseter muscle, one of the chewing muscles in the face. During this surgery, through a small partial facelift incision, the masseteric nerve is removed from its muscle and transferred to the facial nerve branch responsible for innervating the smile muscles. Under an operating microscope, the two nerves are connected using suture finer than a single piece of hair.
Because nerves grow about 1 millimeter a day, we can see the results from this procedure as early as three months after surgery. Because the masseteric nerve was rerouted from the masseter (chewing) muscle and into the facial muscles, clenching down now causes the lower facial muscles to contract – resulting in a fairly natural smile.
Free gracilis muscle transfer
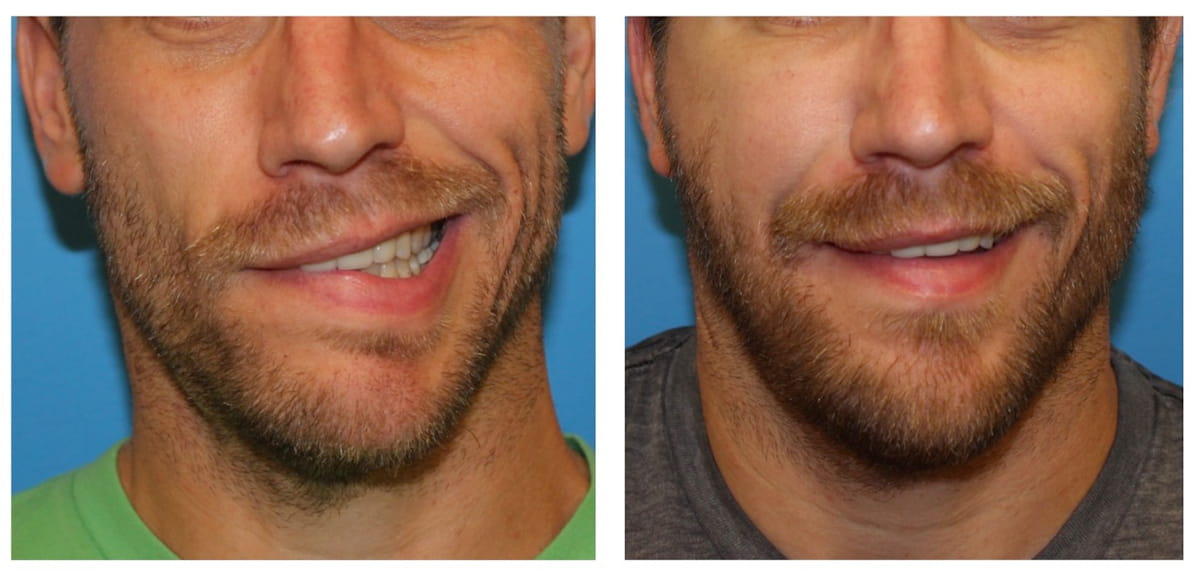 Patients who have had prolonged facial paralysis, in which facial muscles have undergone irreversible atrophy and fibrosis, must have their muscle function replaced. The gold standard procedure for this scenario is called the free gracilis muscle transfer.
Patients who have had prolonged facial paralysis, in which facial muscles have undergone irreversible atrophy and fibrosis, must have their muscle function replaced. The gold standard procedure for this scenario is called the free gracilis muscle transfer.
The gracilis muscle is a thin muscle located in the inner thigh. During this surgery, a portion of this muscle, along with its blood vessels and nerve, is transplanted into the face. After setting the muscle in a vector that is consistent with the smile on the normal side, the gracilis muscle’s blood vessels are connected under a microscope to blood vessels in the neck to allow it to survive. The muscle’s nerve also is connected to a nerve in the face and neck. After about six to 12 months, the nerve grows into the transplanted gracilis muscle, allowing it to move.
Although this is the gold standard, because the native facial musculature and its complex morphology aren’t being used, the smile that results isn’t always perfectly symmetric to the other side. Research is still being done across the world on how to improve these outcomes.
Botox
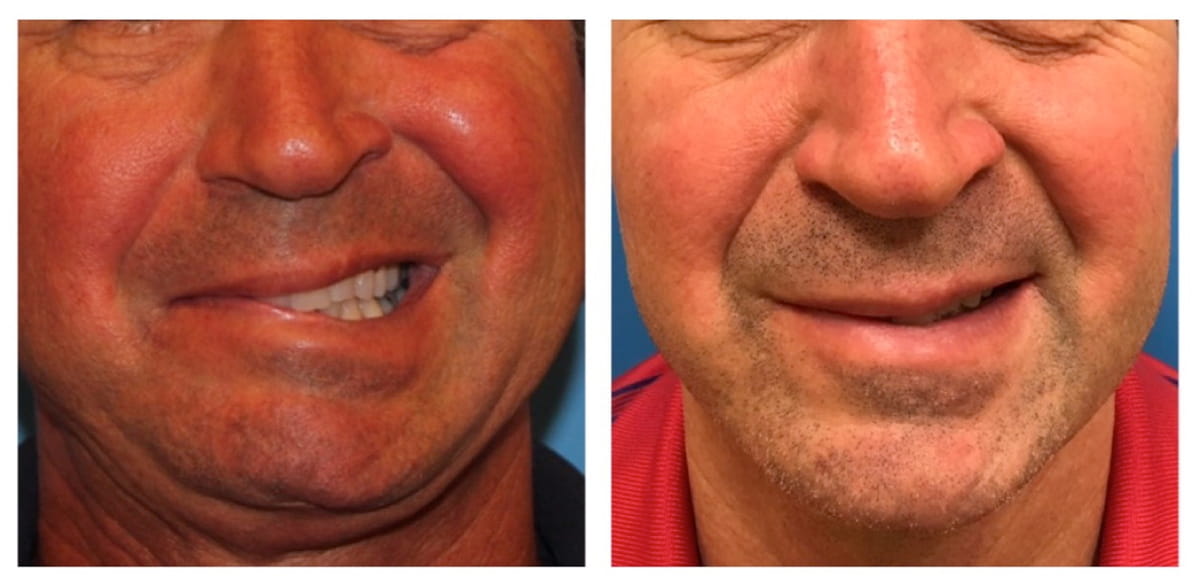 Patients who recover from facial paralysis, such as Bell’s palsy, often develop “synkinesis,” or involuntary facial movements or spasms, that occur during intended voluntary movements. For example, when trying to smile, the muscles that lift the corner of the mouth activate in addition to the muscles that draw the face and the corner of the mouth down. This tug of war distorts the face and often results in a frozen smile.
Patients who recover from facial paralysis, such as Bell’s palsy, often develop “synkinesis,” or involuntary facial movements or spasms, that occur during intended voluntary movements. For example, when trying to smile, the muscles that lift the corner of the mouth activate in addition to the muscles that draw the face and the corner of the mouth down. This tug of war distorts the face and often results in a frozen smile.
Botox is a neurotoxin and temporary muscle paralytic that lasts on average three months. It can be used on the normal side of the face, such as in the forehead and lower lip, to help facial movements appear more symmetric and balanced.
It also can be used in the paralyzed side of the face in patients with synkinesis. For example, for the frozen smile, by selectively paralyzing the down-turning or frowning muscles in the lower face, the smile muscles are better able to exert their action. It helps restore some smile movement and also makes the face less tight and more relaxed.
Dr. Leslie Kim is a facial plastic surgeon at The Ohio State University Wexner Medical Center. Her specialties include aesthetic and reconstructive surgeries of the face and neck, such as facelifts, rhinoplasty, and reanimation after facial paralysis.