September 16, 2021
COLUMBUS, Ohio – The Ohio State University Wexner Medical Center is one of the first in the nation – and the only hospital in Ohio – to use new portable, real-time magnetic resonance imaging (MRI) technology to evaluate and treat stroke patients’ brains at their bedside.
This week the Medical Center’s Comprehensive Stroke Center will start using two FDA-cleared Hyperfine Swoop portable MRI devices in the emergency department and hybrid operating room.
The device assesses brain tissue in real time, which provides physicians the ability to make quick and informed clinical decisions for patients. MRI results are displayed on an iPad and deliver images of the brain tissue within 15 minutes.
 “Portable MRI uses a fraction of the magnetic power that larger conventional MRIs typically use in hospitals,” said Dr. Shahid Nimjee, a neurosurgeon at Ohio State Wexner Medical Center and surgical director of its Comprehensive Stroke Center.
“Portable MRI uses a fraction of the magnetic power that larger conventional MRIs typically use in hospitals,” said Dr. Shahid Nimjee, a neurosurgeon at Ohio State Wexner Medical Center and surgical director of its Comprehensive Stroke Center. “Bringing this technology to the patient’s bedside will allow us to potentially provide more patients with acute treatment for ischemic stroke than is currently available by extending the treatment window for using the clot-busting drug tPA,” said Nimjee, who is also an associate professor in the Ohio State College of Medicine.
Tissue plasminogen activator (tPA) can only be given up to 4½ hours after the “last known well,” which is when the patient was last known to be without the signs and symptoms of the current stroke.
That limits tPA being administered nationally to only about 5% to 7% patients of the 800,000 patients who present with ischemic stroke every year in the United States, Nimjee said.
Because the portable MRI system has a lower field strength than standard MRI systems, this shortens the screening protocol and eliminates the need for comprehensive metal detection, allowing clinicians to rapidly scan, diagnose and treat patients.
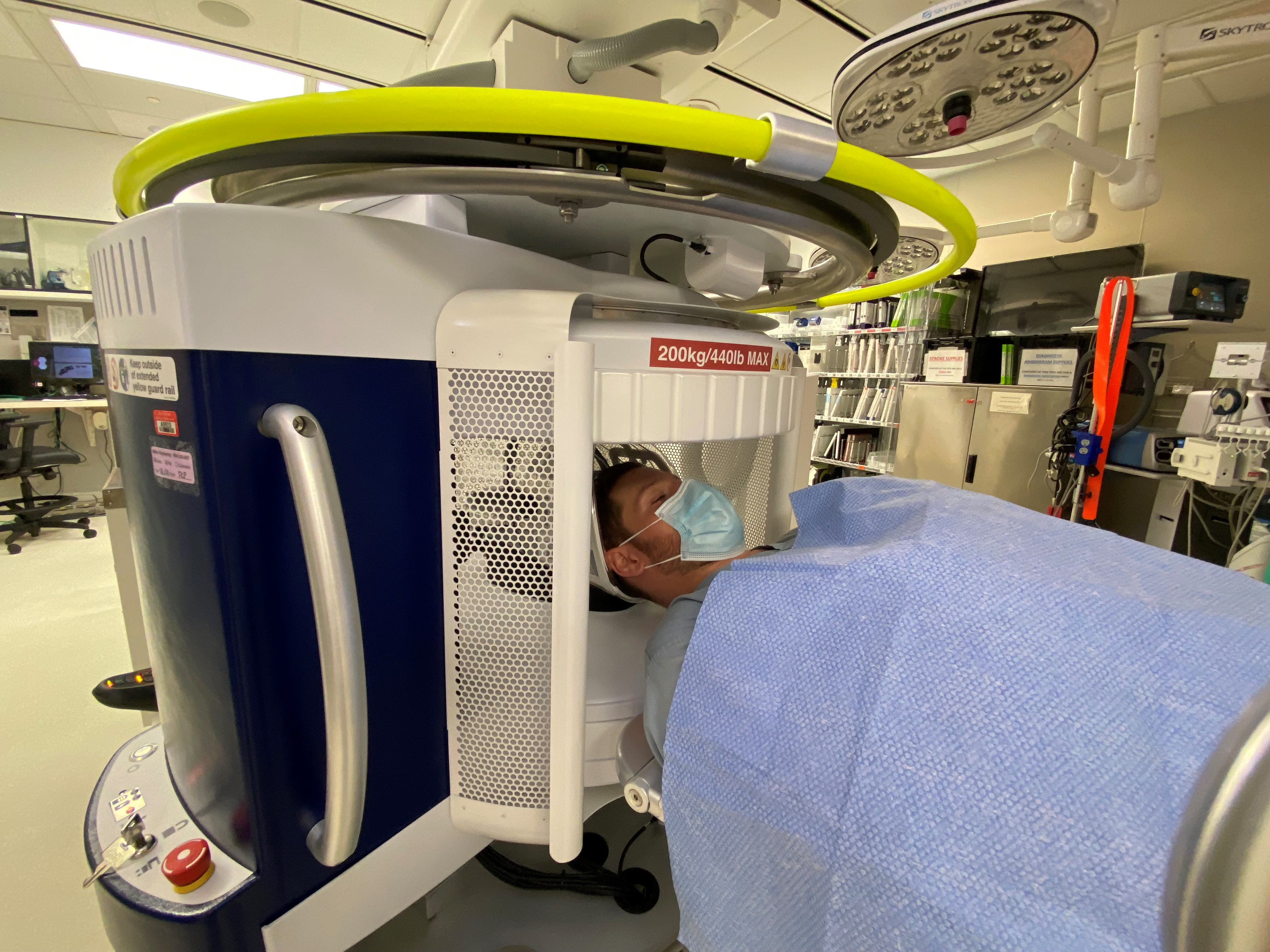
“We simply slide the patient’s head into the head harness and we’re able to take the imaging. As the imaging acquisition happens, it immediately comes into the bed portable screen, so as soon as the imaging has been performed, the neurologist or neurosurgeon can see it, assess the changes and make a clinical decision based on the data in our hands,” said Nimjee, who also is a researcher in Ohio State’s Neurological Institute.
Every 40 seconds, someone in the United States suffers a stroke. It’s the second-leading cause of death worldwide. Most stroke victims don’t receive treatment fast enough to prevent brain damage.
The loss of blood flow that happens during a stroke causes irreversible brain damage resulting in paralysis, speech impairment and loss of motor function.
“Increasing the speed to correlate clinical symptoms with brain tissue imaging will help us provide more patients presenting with acute ischemic stroke with treatment and allow them to return back to functional independence, which is the main goal for our patients,” Nimjee said.
# # #
Media contact: Eileen Scahill, Wexner Medical Center, Eileen.Scahill@osumc.edu
