September 12, 2016
 COLUMBUS, Ohio – The Ohio State University Wexner Medical Center’s Comprehensive Transplant Center is the first in Ohio and among only a handful nationwide to test a novel method that could potentially double the number of available lungs for transplantation and save more of the 35 million Americans suffering from chronic lung disease.
COLUMBUS, Ohio – The Ohio State University Wexner Medical Center’s Comprehensive Transplant Center is the first in Ohio and among only a handful nationwide to test a novel method that could potentially double the number of available lungs for transplantation and save more of the 35 million Americans suffering from chronic lung disease.As central Ohio’s only adult transplant center and with one of the country’s largest transplant programs in the U.S., Ohio State’s Wexner Medical Center is one of 17 institutions across the country certified to evaluate the safety and effectiveness of Ex-Vivo Lung Perfusion (EVLP) through participation in the NOVEL extension clinical trial.
“Expanding the number of lifesaving and life-enhancing lung transplants is limited by the number of available donors and the quality of the donated organs. Having the ability to more adequately evaluate potential donor organs and to even repair or resuscitate them is a game changer for lung transplantation,” said Dr. Bryan Whitson, a cardiothoracic surgeon and director of the lung transplant program at Ohio State’s Wexner Medical Center.
EVLP treatment assesses the viability of donated lungs for transplantation to expand the donor (lung) pool, improve the function of donated lungs that might otherwise be considered unsuitable for transplantation and decrease inflammation and rejection for the lung transplant patient.
“In addition to being able to rescue lungs not traditionally transplantable, EVLP provides us with an opportunity to begin to more actively and routinely repair organs in the next couple of years,” said Whitson, also principal investigator of the study at Ohio State.
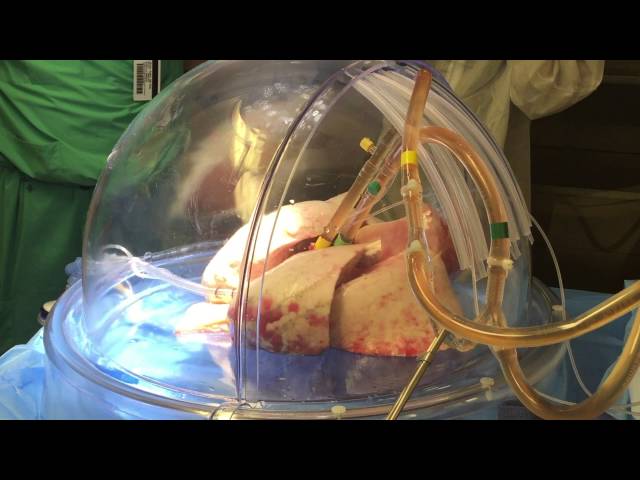
Once donated lungs are acquired from a deceased organ donor, the EVLP process begins with placing donated lungs inside a sterile plastic incubator-like dome and attaching them to a circuit, which includes a ventilator, perfusion pump and filters. The lungs are maintained or supported on the circuit at normal body temperature and perfused with a bloodless solution containing nutrients, antibiotics and oxygen, which can repair injured lungs and remove excess water.
During the three to six-hour perfusion process, lung function is consistently monitored against key indicators, such as oxygen exchange, airway pressure and lung compliance. If lungs are deemed suitable after EVLP treatment, they are immediately transplanted into a waiting lung transplant patient.
“If all goes well, our hope is to ultimately increase recovery of suitable lungs enough to where we could essentially take all those anxiously awaiting a lifesaving lung transplant off the waiting list,” Whitson said.
Each year, less than 2,000 lung transplants are performed in the U.S., as lungs are the most fragile organs to transplant and fewer than 30 percent of all donor lungs meet the criteria for transplantation.
Ohio State’s Comprehensive Transplant Center has performed more than 8,500 lifesaving transplants in almost 50 years, including lung, heart, heart-lung, kidney, living donor kidney, liver, pancreas and kidney-pancreas transplants.
###
Contact: Sherri Kirk, Wexner Medical Center Public Affairs and Media Relations, 614-293-3737, or Sherri.Kirk@osumc.edu.