The 5 Cs of choosing an insulin delivery method
 For people with diabetes, insulin is a life-saving medication. Those with Type 1 diabetes can’t survive without it, and many people with Type 2 also need it. In the nearly 100 years since insulin was first discovered as a treatment, we’ve come a long way in how people use it. There are many forms and many ways to get it into the body.
For people with diabetes, insulin is a life-saving medication. Those with Type 1 diabetes can’t survive without it, and many people with Type 2 also need it. In the nearly 100 years since insulin was first discovered as a treatment, we’ve come a long way in how people use it. There are many forms and many ways to get it into the body.
When I talk with patients about choosing the best insulin delivery option for them, there are 5 Cs I review:
Choice
It used to be that patients had to inject themselves with insulin from a syringe. Not anymore. While that’s still a great option for some people, others can take advantage of newer forms such as pens, pumps, a patch-like device and an inhaler.
Pens gained popularity about 15 to 20 years ago and they’re widely covered by insurance. They still require the patient to inject the medication, but it’s more portable, more accurate and much easier to dose.
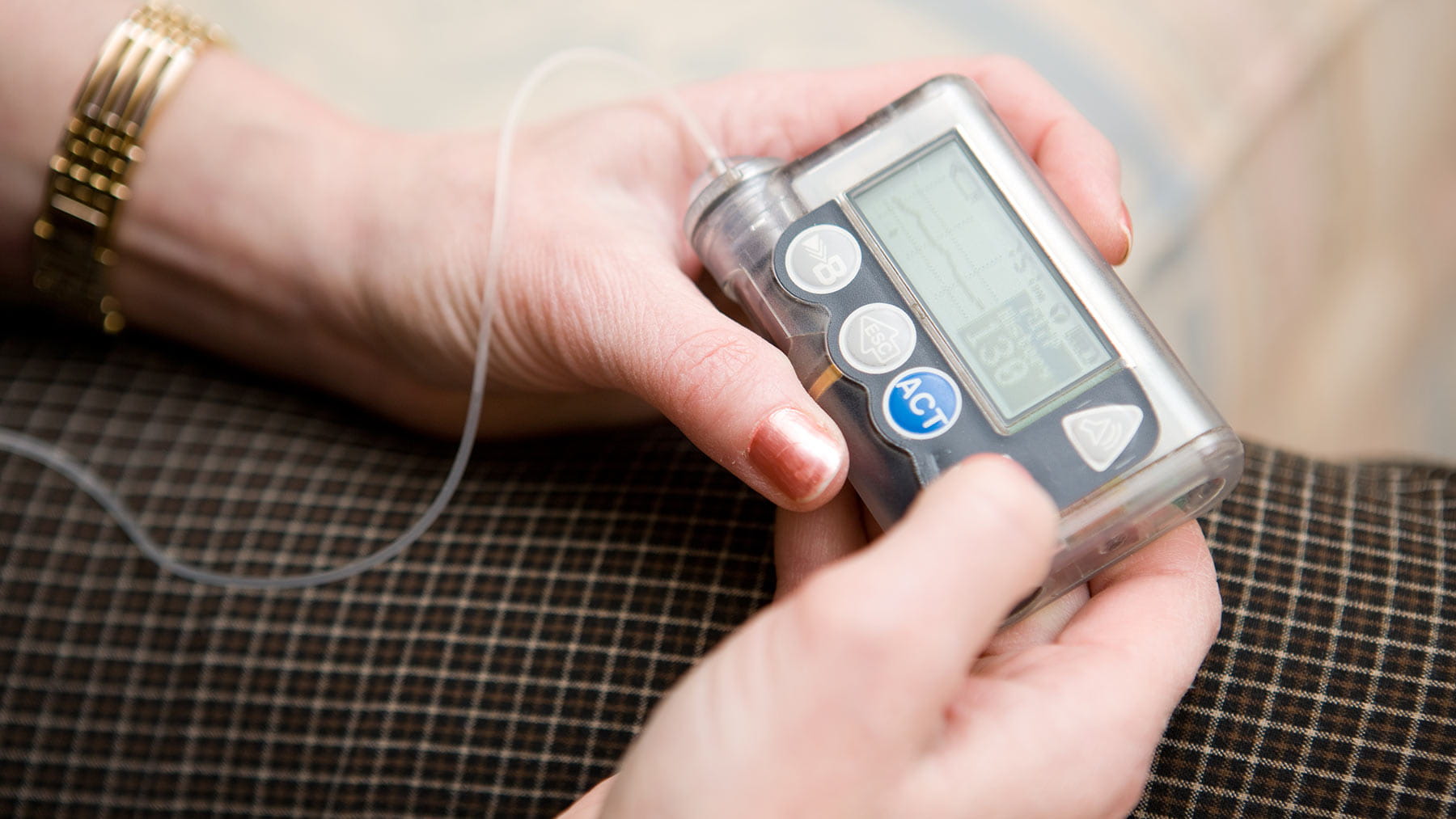
There are three insulin pumps currently available. Pumps continuously deliver insulin from a small cannula, or thin tube, under the skin. This is changed every two to three days. They can be programmed to dose insulin when eating, or to adjust amounts for exercise and other variations in lifestyle. New versions have combined a pump with glucose sensing to make blood sugar control even easier. While pumps are generally used more by people with Type 1 diabetes, about 20% of our patients with Type 2 use this technology.
Another option is similar to a pump, worn like a patch and changed every 24 hours. A tiny needle goes under the skin to deliver insulin continuously. Insulin can be delivered for meals with a simple click.
There is also an inhaler that delivers fast-acting insulin before meals. It’s very similar to the inhaler people with asthma use. Patients breathe a fine insulin powder into the lungs. However, it’s not for people with asthma or a history of smoking in the last six months.
Cost
This is obviously a big concern for most patients who must manage diabetes for life. Lately the cost of insulin has skyrocketed, leading some patients to try self-rationing to make their supplies last longer. This is dangerous and can cause serious and even life-threatening problems.
Vials and syringes are the most cost-effective way to go. Syringes are cheap and a vial of insulin contains 1,000 units. Each pen holds about 300 units and it’s discarded, so there is more expense to produce it.
Talk with your insurance company or pharmacist to know which insulin they’ll cover. Compare pharmacies for the best price possible.
Convenience
While it’s more expensive than ever, taking insulin can also be more convenient than ever. Today’s insulin delivery is more comfortable because the needles are smaller and thinner.
Depending on the method, it can be pretty subtle. For example, no one will notice an insulin pump worn under clothing. Even a pen injection can be discrete. New glucose monitors also reduce the need for frequent finger sticks.
Consistency
It’s important to choose an insulin delivery method that helps you be consistent. High and low blood sugar have bad complications on all your organs, so the more time you spend in the healthy range, the better.
A pump is the most precise and most accurate method because you get smaller and more frequent doses, more like how the body works. Pumps take the math and guessing away. People on insulin pumps have far fewer episodes of low blood sugar or accidental overdosing of insulin.
Pens and vials of insulin rely more on the user. As long as you’re consistent and doing the math, they can work well. With vials and syringes, a small air bubble could throw off the dose. With these methods it’s also easier to miss a dose. Many patients miss at least once a week.
Challenges
There are various challenges to using insulin. This medicine is sensitive to temperature and light. As a protein, it breaks down in extreme heat or cold, therefore keep vials in the original box and cap the pens when not in use.
Many patients use both short- and long-acting forms of insulin. Nowadays most insulin is clear, making it very easy to mix them up. I tell people to store their insulin separately or use different forms, such as a pen for one and a vial/syringe for the other.
Pump safety is a concern right now. Pumps are the leading FDA-reported device for fatalities. They can also be a little overwhelming to set up. Even for experienced pump users, errors can happen when entering settings in a new pump. We highly recommend working with a certified pump trainer when setting up a pump. Most people new to insulin start by using pens.
Another challenge is disease fatigue. It can be tiring to constantly monitor diet and blood sugar. Even a pump doesn’t allow you to ‘set it and forget it.’ Vigilance will always be key.
Insulin is the most powerful, most precise drug we have for diabetes. With power, you have to understand and respect how to use it. Talk with your doctor or a certified diabetes educator to help you make the decision that’s best for you and your lifestyle.
Janet Zappe is a certified diabetes educator with The Ohio State University Wexner Medical Center.