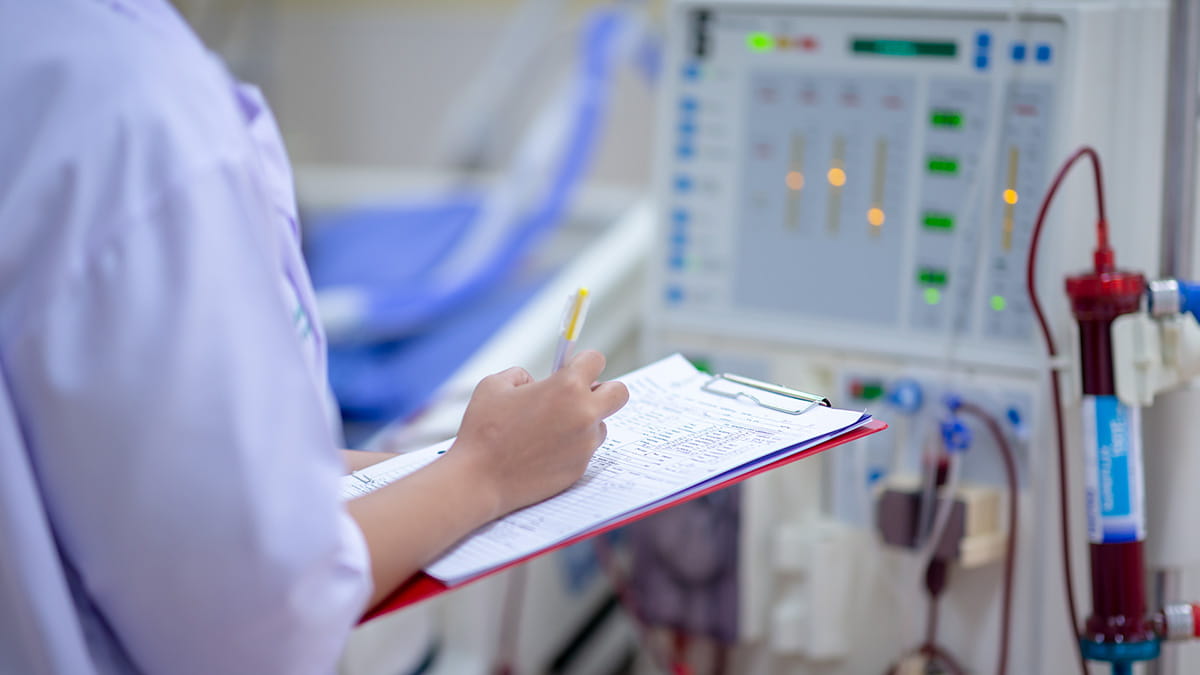
Pig kidneys in humans? Such breakthroughs could shorten wait lists for transplants
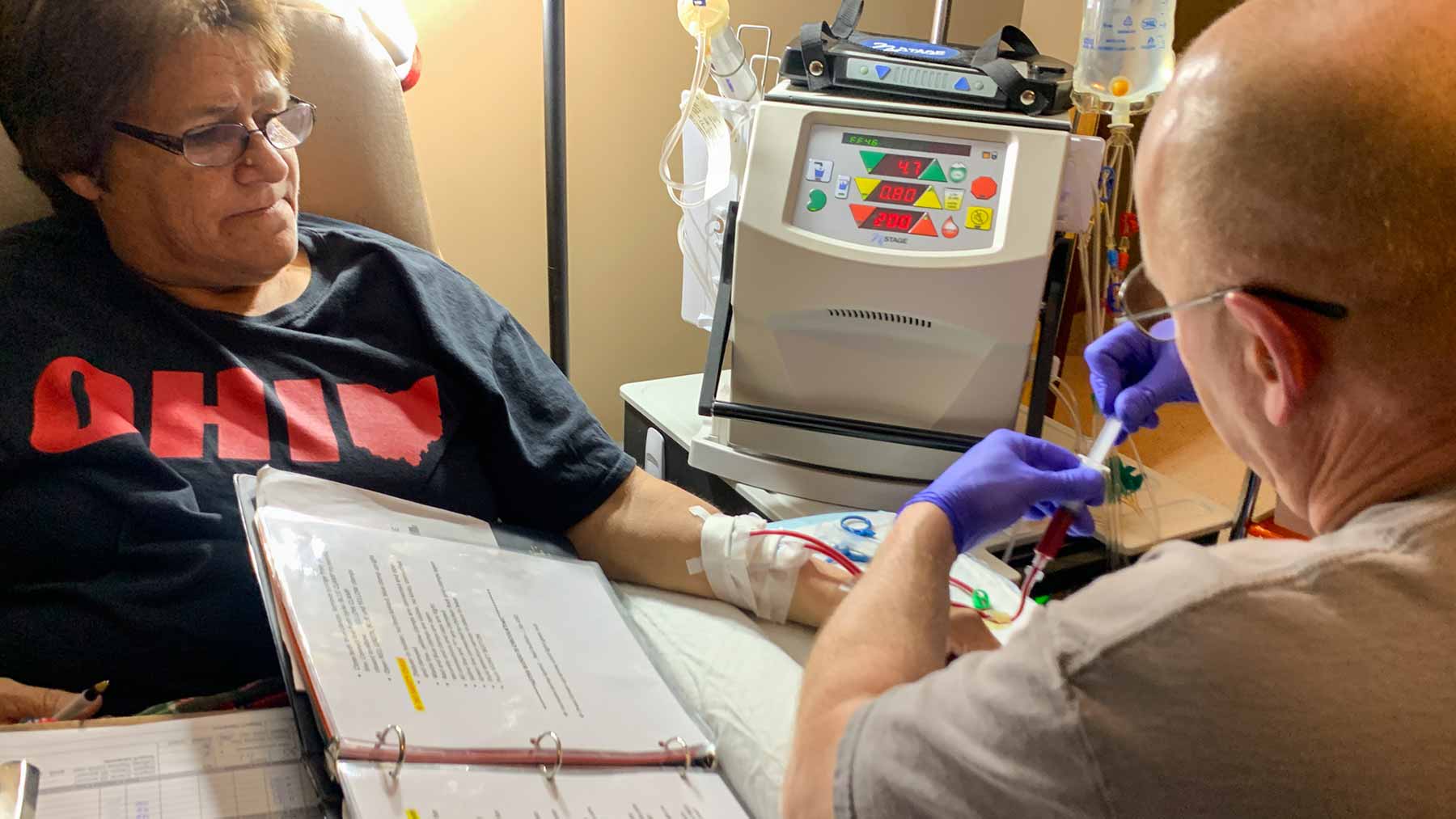
More organ transplants were performed last year than ever before, and while the success rate of these lifesaving procedures continues to improve, about one in four patients develops antibodies that can cause rejection, organ failure or even death months or years after surgery. Now, researchers at The Ohio State University Wexner Medical Center have discovered a new type of immune cell that predicts a transplant patient’s risk of rejection and may lead to therapies that reduce their risk.
“This specific type of antibody can cause immediate damage to the organ or long-term graft rejection, which means that the patient’s organ is not going to last as long,” said Dr. Ginny Bumgardner, transplant surgeon at The Ohio State University Wexner Medical Center and lead author of the study. “This cell type that we studied was very interesting because it had the capacity to reduce antibody production in transplant recipients.”
The study measured levels of the cell in patients’ blood throughout the first year following kidney transplant surgery and found that those with higher levels of the cell were less likely to develop donor-specific antibodies. Bumgardner says this not only could help doctors assess a patient’s risk of rejection, but she hopes it will also lead to new treatment options before and after surgery.
“These cells may be used to prevent antibody development in the first place, and they may also be used to suppress antibodies for those patients who develop them after surgery,” Bumgardner said.
If experts are able to grow these cells in a lab and deliver them to transplant patients, it could reduce or eliminate the need for immunosuppressive therapies that are not always effective and put patients at a higher risk of infection and other health issues. Preventing organ rejection can also reduce the need for additional transplants, which will help alleviate the organ shortage for the more than 110,000 Americans waiting for a lifesaving transplant.
Watch the video below to learn more about this research.