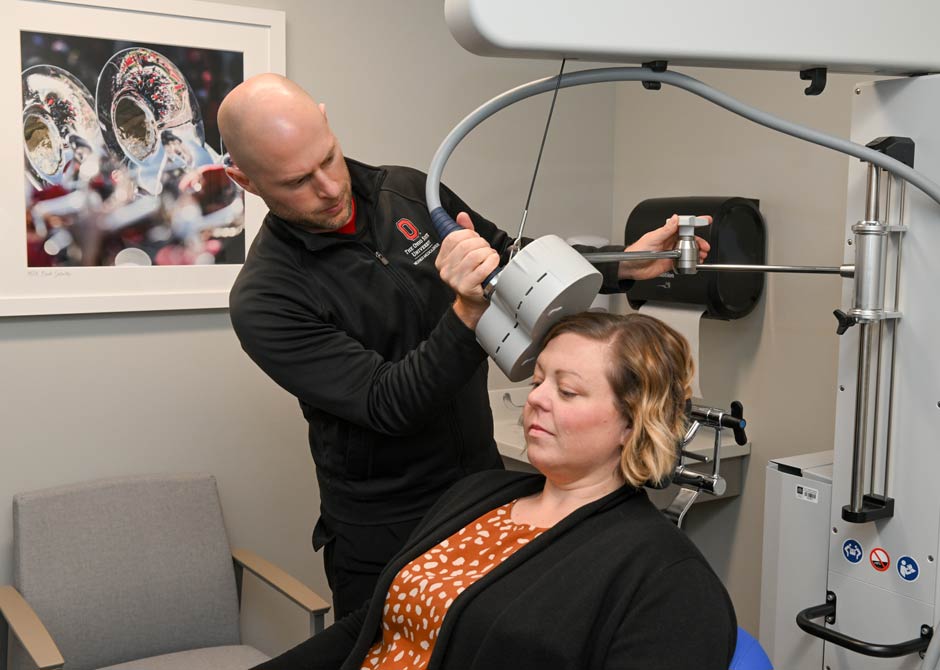
 Transcranial magnetic stimulation is a non-drug treatment for depression and other conditions that uses magnetic pulses to stimulate areas of the brain to influence mood. It’s noninvasive and often used when other, more common forms of mental health treatment — such as medications or psychotherapy — have not worked well enough to treat your condition.
Transcranial magnetic stimulation is a non-drug treatment for depression and other conditions that uses magnetic pulses to stimulate areas of the brain to influence mood. It’s noninvasive and often used when other, more common forms of mental health treatment — such as medications or psychotherapy — have not worked well enough to treat your condition.
TMS is one of the many therapies the mental and behavioral health experts at The Ohio State University Wexner Medical Center in Columbus, Ohio, can prescribe to improve your symptoms and quality of life.
If you or a loved one is suffering from severe depression or other worsening mental health conditions, you might want to consider undergoing TMS. Our mental health experts excel at identifying candidates who will benefit the most from TMS, and we’ll work with you to decide if it should be part of your personalized treatment plan. Each person we treat for a mood disorder undergoes a thorough evaluation to determine which treatments will be the most effective.
What is TMS therapy?
Transcranial magnetic stimulation, which is approved by the U.S. Food and Drug Administration, stimulates areas of the brain that are thought to control mood. This is done through brief magnetic pulses. These pulses are generated by an insulated coil placed on the scalp, and they pass through the skull to the brain.
The therapy treats depression and mood disorders and is typically reserved for people whose conditions have not responded to traditional treatments. It’s an important tool for mental health professionals since depression affects 1 in 6 Americans, and conventional treatments, like medications and talk therapy, are not sufficiently effective for some people.
Why is transcranial magnetic stimulation done?
Typically, TMS isn’t the first line of treatment that providers recommend for certain mood disorders and other mental health conditions. It’s often a treatment that can help when other treatments have not worked adequately enough.
Conditions that can be treated by TMS include:
How does TMS work?
With TMS, brain areas that are overactive can be slowed, and brain areas that are underactive can be stimulated. People with depression tend to have brain areas that are underactive. Once those areas are stimulated, a person will begin to feel better.
It’s not entirely understood why TMS relieves these depressive symptoms, but it’s been shown to cause changes in the neuronal activity in the areas of the brain responsible for mood.
Our TMS sessions, which last less than an hour, are typically scheduled five days a week for approximately four to six weeks, but your regimen can vary based on your condition and needs. It’s personalized to your unique situation.
Benefits of transcranial magnetic stimulation
TMS has various benefits for those suffering from debilitating depression. Those benefits include:
- It’s noninvasive. TMS is done as an outpatient procedure, meaning you go home the same day.
- It has fewer side effects. Other treatments for depression, like medications, can have uncomfortable side effects. TMS is well tolerated
- It works. TMS has been studied in people who haven’t benefitted from other treatments and can help even in those cases
- It can be used alongside other therapies. People can still use medications, psychotherapy and other treatments while undergoing TMS.
What to expect during TMS?
 It’s important to remember that our mental health specialists most likely won’t recommend TMS as the first therapy to try. Usually, we’ll want to see how you respond to antidepressants or talk therapy if you haven’t already used those treatment methods.
It’s important to remember that our mental health specialists most likely won’t recommend TMS as the first therapy to try. Usually, we’ll want to see how you respond to antidepressants or talk therapy if you haven’t already used those treatment methods.
You’ll be given an initial evaluation to assess your condition, and we’ll discuss the risks, benefits and alternatives to treatment with you before you start the procedure. The following conditions might disqualify you from TMS:
- You’re pregnant.
- You have a metal or implanted device in your body, including aneurysm coils, pacemakers, cochlear implants, stimulators or bullet fragments.
- You have seizures.
- You have a traumatic brain injury.
- You’re on certain medications.
If you and your doctor decide TMS might be beneficial, here’s what will happen:
Before the procedure
TMS is an outpatient procedure, meaning you won’t be under general anesthesia or need to stay at the hospital. You can drive yourself home, but some people prefer to have someone else transport them in case they experience mild side effects.
Your doctor will also talk to you about the TMS regimen that might be most beneficial for you.
During the procedure
You’ll come to one of Ohio State’s outpatient treatment facilities. You’re awake and alert during the treatment. Here are the steps to the procedure:
- You’ll remove glasses and any jewelry as a precaution.
- You’ll sit in a specially designed chair, and you’ll be given ear plugs to protect your ears.
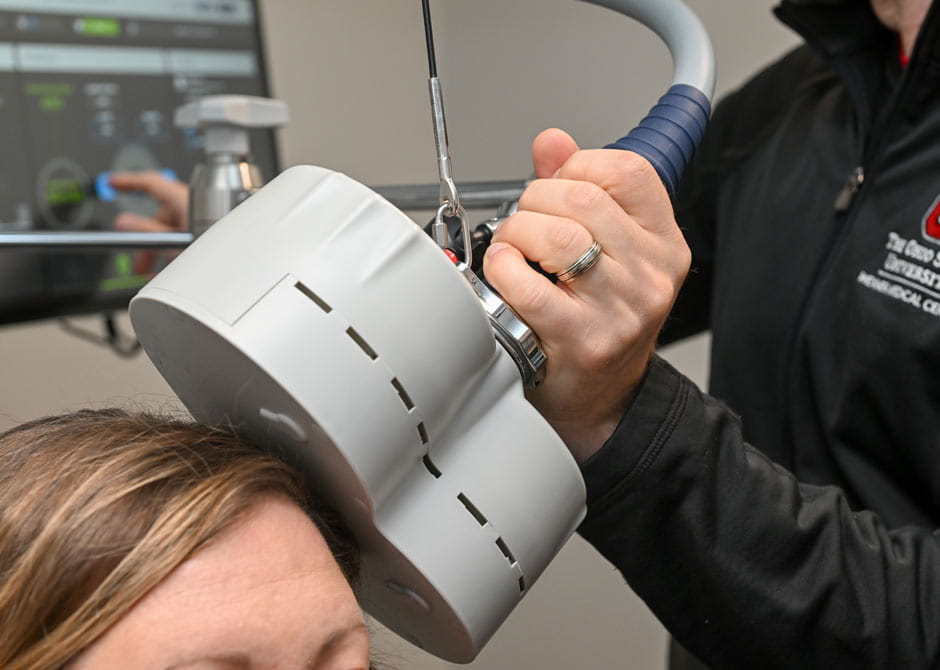
- A magnetic coil, which will be in a helmet or other device, will be placed on your head.
- Once the magnet is turned on, you’ll hear a repeated tapping followed by a pause.
- During your first treatment, the coil will be moved around your head to find the spot where the magnetic pulses cause your hands to twitch on the opposite side of your body. In subsequent sessions, the coil will be placed in that spot.
- Depending on your condition, the pulse patterns can last anywhere from a few minutes to half an hour.
Results of TMS
People are usually able to resume normal activities following transcranial magnetic stimulation. Some people may notice an improvement in their depression as early as the first or second week of treatment. Most people will find that symptoms improve gradually during the weeks of treatment.
What are the risks of transcranial magnetic stimulation?
TMS is a well-tolerated procedure that has been studied and improved over several decades. However, just like with most medical interventions, there are always some risks, even if rare.
The most severe risk of TMS is a seizure, but that happens in only 0.01% of cases, or 1 in 10,000 procedures.
Other common side effects last only a few minutes after the procedure. They include:
- Headaches
- Dizziness
- Pain in scalp or neck
- Hearing issues, such as tinnitus (ringing in ear) or sound sensitivity
- Tingling in face or head
How to get a referral?
To begin the initial evaluation process to find out if transcranial magnetic stimulation is right for you, call our mental health specialists at 614-293-8552.

 Transcranial magnetic stimulation is a non-drug treatment for
Transcranial magnetic stimulation is a non-drug treatment for  It’s important to remember that our mental health specialists most likely won’t recommend TMS as the first therapy to try. Usually, we’ll want to see how you respond to antidepressants or talk therapy if you haven’t already used those treatment methods.
It’s important to remember that our mental health specialists most likely won’t recommend TMS as the first therapy to try. Usually, we’ll want to see how you respond to antidepressants or talk therapy if you haven’t already used those treatment methods.

