At The Ohio State University Wexner Medical Center in Columbus, Ohio, our comprehensive team of specialists is dedicated to helping you improve your hearing and communication.
If you struggle with hearing loss and have been dissatisfied with your experience with hearing aids, it may be time to determine whether you’re a candidate for cochlear implants, which are internal electronic devices that can improve hearing. People who have severe hearing loss from inner-ear damage but don’t respond well to traditional hearing aids could benefit from these remarkable devices.
An audiologist in our nationally ranked ear, nose, and throat (ENT) department can conduct a series of tests — a hearing test, a physical exam and a cochlear implant evaluation — to determine your possible compatibility with cochlear implants.
The adult cochlear implant program at the Ohio State Wexner Medical Center has been assisting patients with hearing loss for more than 25 years. The goals of our program are simple: provide the most outstanding and comprehensive hearing care, while advancing the ever-evolving field of cochlear implantation through research and innovation.
What is a cochlear implant?
A cochlear implant is a device that can help you hear when hearing aids are either not powerful enough or don’t make speech clear enough in conversation. There are two parts to the device:
- an internal portion that is placed during outpatient surgery
- an external processor that is programmed a few weeks after the surgery
The external processor captures sound from the environment, processes the sound into digital information and sends this data to the electrode array inside the cochlea (the inner ear).
The cochlear implant helps with speech recognition, enabling those with significant hearing loss to communicate more effectively. Learning to properly utilize the cochlear implant after surgery usually takes three to six months.
How does a cochlear implant work?
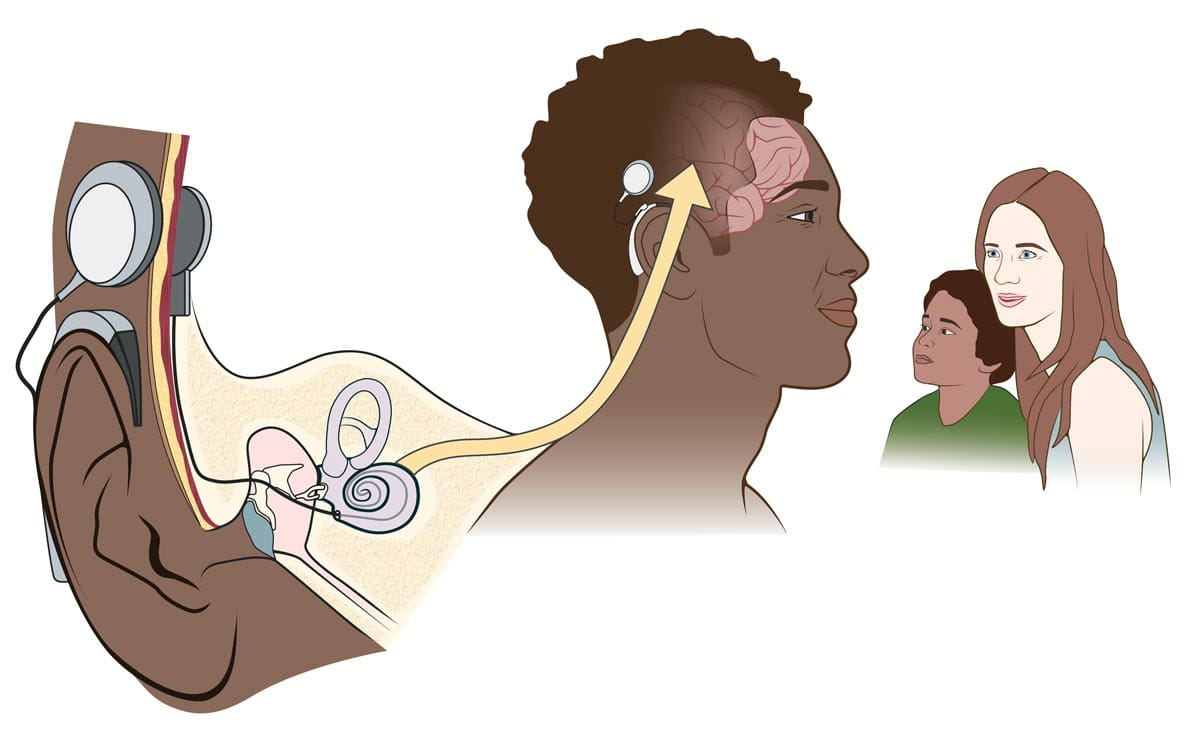
A cochlear implant works by stimulating the auditory nerve directly, bypassing any damage in the inner ear. The external processor worn behind the ear converts sound into electrical signals. These are then sent through a coil behind the ear and into a receiver implanted in the skull. From there, the signals are processed by electrodes placed around the cochlea, stimulating auditory nerve fibers to send signals to the brain.
Benefits of cochlear implants
Getting cochlear implants can be a life-changing experience. People who use them have often tried other hearing devices with little success and this technology offers people with hearing loss the opportunity to engage socially in ways not possible before.
Many cochlear implant users report feeling more connected to family, friends and environments, allowing them to work and build relationships more effectively. Confidence and independence are often gained through this procedure.
Differences between cochlear implants, bone conduction devices and hearing aids
Traditional hearing aids are often the first step to improving hearing. The amplified signal can be tailored to specific pitches and amount of amplification needed based on each person’s hearing loss. Bone conduction devices are used in people with single-sided deafness or chronic ear problems, such as draining ears that make wearing traditional hearing aids impossible. These devices can bypass the portion of the ear that is not functioning to stimulate the healthy inner ear.
Cochlear implants are used in people when hearing aids are no longer helpful. The internal device directly stimulates the auditory nerve bypassing the inner ear.
What to expect during cochlear implant surgery
Cochlear implant surgery is considered a simple and safe procedure, and many people who undergo it experience improvements in what they’re able to hear.
Preparing for cochlear implant surgery
You’ll meet with members of our multidisciplinary team to determine if you are a candidate for surgery. This will include seeing:
- an audiologist who will test your hearing abilities, with and without hearing aids
- a surgeon who will determine if a cochlear implant is medically appropriate
It generally takes two visits before you’re medically cleared for surgery. You and your doctors will discuss how the decision to get a cochlear implant is a lifechanging one that will require dedicated effort from you to learn to use the implant.
During a cochlear implant surgery
The surgery itself typically takes one to two hours, and you’ll be under general anesthesia.
Your surgeon will make a small cut behind your ear and create a hole in the skull bone, called the mastoid, where the device will be placed. Then, the surgeon will thread the electrode of the internal device through a small opening in the cochlea. Finally, the skin incision is stitched closed.
Activation of the device will be performed approximately three to four weeks later.
Cochlear implant surgery recovery and follow up
After the surgery, you can expect some mild discomfort for a few days, but this should be managed with pain medications. The incision will remain bandaged for about two weeks.
Once you’ve recovered from the implantation surgery, you will have an appointment with your audiologist to program the device. From there, you’ll begin to learn how to recognize sounds. This process will require routine use of the cochlear implant as well as your willingness to engage in listening opportunities and an overall commitment to return for follow-up appointments.
Your family will also play a vital role. Here’s what the process might look like:
- Device activation a month after surgery where your audiologist will help you determine goals
- A care plan with several follow-up appointments to adjust the external processor and implement guided listening training
- Learning opportunities to understand the technology and accessories
- Initial hearing rehabilitation lasting three to four months
- Annual visits following the adjustment period
With time, practice and patience, many recipients notice an improvement in their ability to participate in conversation compared to their preoperative performance with hearing aids.
Patient Forms
Additional Information
How would you like to schedule?
Don’t have MyChart? Create an account
















