 What is a herniated disc?
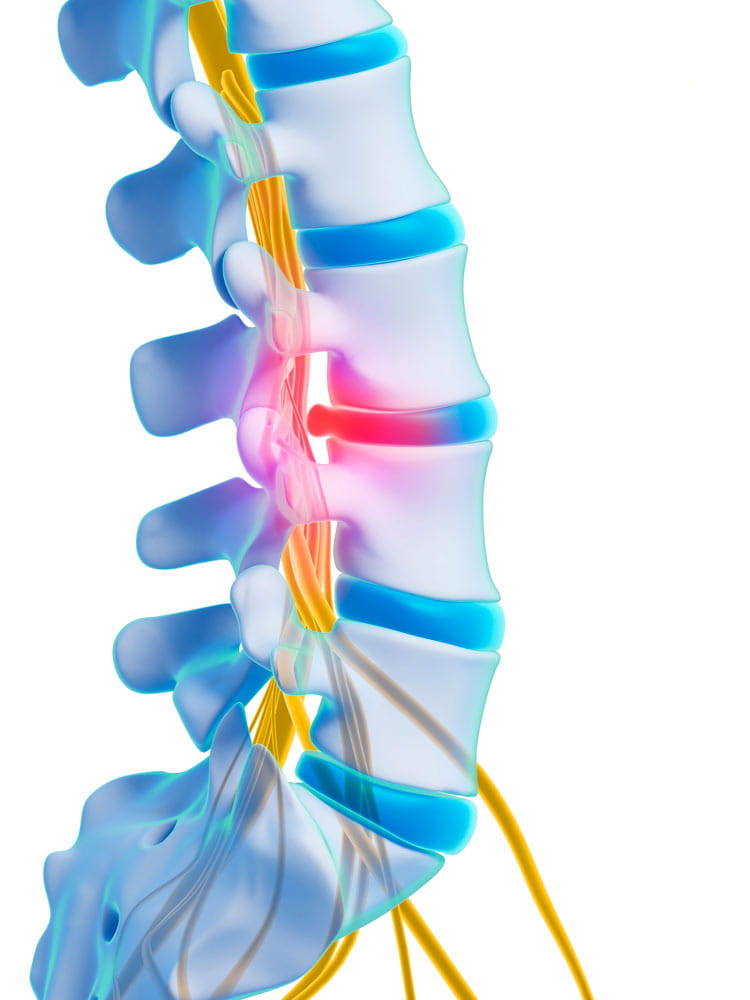
What is a herniated disc?
Your backbone, or spine, is made up of 26 bones called vertebrae. In between them are soft discs filled with a jelly-like substance. These discs cushion the vertebrae and keep them in place. As you age, the discs break down, or degenerate. As they do, they lose their cushioning ability, which can lead to pain if the back is stressed.
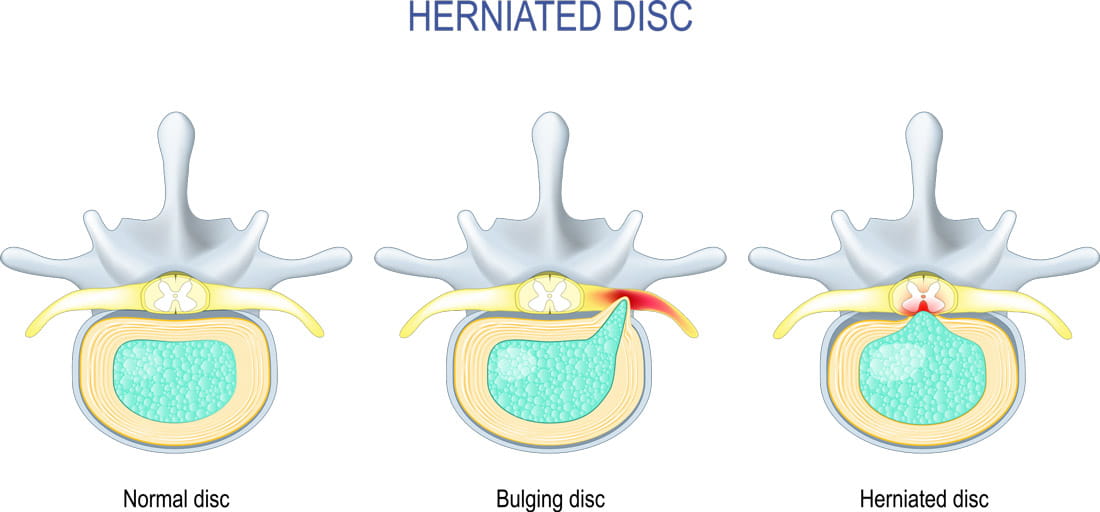
A herniated disc is a disc that has ruptured or torn. This allows the jelly-like center of the disc to leak, irritating the nearby nerves. A herniated disc can occur anywhere along your spinal column, though most often in the neck (cervical) or low-back (lumbar). If the bulging disc is pressing on a nerve, it will send shooting pains to the area connected to that nerve — commonly called a pinched nerve.
A herniated disc in the upper or lower spine could weaken muscle groups in the arm or leg. The upper-back discs of the thoracic spine could cause problems to the bladder or bowel, or shooting pains toward one side of the body.
Your doctor will diagnose a herniated disc with a physical exam and, sometimes, with imaging tests. Most people recover with treatment, which includes rest, anti-inflammatory and pain medicines, physical therapy and, sometimes, surgery.
At The Ohio State University Wexner Medical Center, our team of neurological and orthopedic experts are ready to fix your herniated disc.
What causes a herniated disc?
Herniated discs are typically caused by wear and tear. Several factors can contribute to the formation of a herniated disc, including:
- Aging – as we age, the discs in our spines lose some of the fluid that helps them stay flexible
- Having excessive weight
- Overuse with repetitive motion
- Injury or strain causing the jelly-like material inside the disc to be forced out through tears or cracks, which leads to the disc bulging or breaking into fragments
Herniated discs also are more common in people who smoke.
Herniated disc symptoms
Symptoms of a herniated disc vary depending on their location in your spine. Most occur in the lower back (lumbar herniated discs) or neck (cervical herniated discs).
Lumbar herniated disc symptoms
- Leg pain – this sciatic nerve pain shoots down one side of your buttocks, thigh and into your leg or foot
- Numbness or tingling in the legs or feet
- Muscle weakness
Cervical herniated disc symptoms
- Pain between your shoulder blades
- Pain that radiates to your shoulder, arm, hand or fingers
- Pain in the sides or back of your neck
- Numbness or tingling in your arms or legs
- Neck pain that increases when turning your head
Seek medical attention right away if you have weakness or numbness in both legs along with a loss of bladder and/or bowel control as it could be a sign of a rare but serious issue called cauda equina syndrome.
Diagnosing herniated discs
Your doctor may determine you have a herniated disc with a combination of a physical exam and imaging tests, such as:
- X-rays
- Magnetic resonance imaging (MRI) scan
- Computed tomography (CT) scan
- Electromyography study (EMG), a test that measures the electrical activity of muscles
- Nerve block to identify the specific nerve irritated by a herniated disc
Herniated disc treatment
 For most people, time and rest will fix a herniated disc. Some people may need additional treatment.
For most people, time and rest will fix a herniated disc. Some people may need additional treatment.
Ohio State offers a wide variety of treatment for herniated discs ranging from physical therapy to the most complex neck and spine surgeries. Because 90% of herniated discs get better on their own, our specialists start with less invasive options, including lifestyle changes and nonsurgical treatments, before recommending surgery. Our spine specialists have several recommendations to increase mobility and reduce pain:
Lifestyle changes
Adjusting your daily habits may prevent future herniated discs. Those changes may include:
- Strengthening back muscles through exercise, including Pilates or yoga
- Practicing good posture
- Maintaining a healthy weight
- Using proper lifting techniques
- Quitting smoking
At-home treatment of herniated discs
- Rest for a few days – but also move around occasionally to prevent stiffness
- Appy ice or heat to affected area
- Take over-the-counter medication for pain, such as ibuprofen or acetaminophen
Nonsurgical treatment options
- Physical therapy
- Acupuncture
- Anti-inflammatory medication or muscle relaxers
- Spine orthobiologics
- Spinal injections, including corticosteroids, for pain or nerve blocking
- Real-time ultrasound imaging (RUSI) of movement in the spine area to retrain the deep stabilizing musculature of your spine (a highly researched, evidence-based intervention)
Surgery to treat a herniated disc
If nonsurgical treatments are unsuccessful, your doctor may give you options for surgical procedures to address your herniated disc. Depending on your specific needs, your doctor may recommend:
- Artificial disc surgery/replacement
- Microdiscectomy/discectomy – the removal of a damaged portion of a herniated disc in the spine
- Laminectomy – the removal of part of the bone around a herniated disc and expansion of your spinal canal
- Spinal fusion – directly joining two or more vertebrate to provide stability
Microdiscetomy surgery
We perform minimally invasive surgery (using small incisions, working through a tube) only if the disc is causing severe weakness, pain that does not improve over time or loss of mobility.
Research
For those who are experiencing a herniated disc, you may be eligible for one of the following areas of research focus at Ohio State:
Biomechanical testing: We’re using biomechanical testing to judge the spine before and after surgery. A specialized vest assesses your spinal movement and measures the effectiveness of surgery. It ultimately may provide valuable information about which treatments will best increase mobility and function of the spine.
Back pain consortium: We’re part of the International Consortium for Health Outcomes Measurement (ICHOM). This allows us to engage with other top U.S. medical centers in global research studies on back pain. As we measure our results against established international standards, we share best practices and elevate our standard of care.
How would you like to schedule?
Don’t have MyChart? Create an account

