Heart arrhythmia
An arrhythmia, sometimes referred to as an irregular heartbeat, is an abnormal rhythm of the heart, which can cause the heart to pump less effectively. The heart may pump too fast, too slow or irregularly.
At least 2.7 million Americans have atrial fibrillation, the most common rhythm disorder, and the number is expected to double in the next 30 years.
As one of the top programs in the nation treating heart rhythm disorders, Ohio State offers cutting-edge care to treat arrhythmias:
- Ablation procedures
- Device implants, such as pacemakers and defibrillators
- Medications
- Minimally invasive procedures that improve the accuracy and precision of treatment
- Surgical procedures
We are the only hospital in central Ohio and one of the first heart and vascular centers in the world to do rotor mapping of atrial fibrillation for ablation of rotors in the heart, using focal impulse and rotor modulation (FIRM) guided therapy.
Physicians who treat heart rhythm disorders are known as electrophysiologists. The Electrophysiology team at Ohio State Richard M. Ross Heart Hospital consists of the largest group of electrophysiologists in central Ohio, as well as more than 100 nursing staff members dedicated to the care of patients with arrhythmias.
Arrhythmia types
There are different kinds of arrhythmia or irregular heartbeats. When the heartbeat is too slow (fewer than 60 beats per minute), it’s called bradycardia or bradyarrhythmia. When the heartbeat is too fast (more than 100 beats a minute), it’s called tachycardia or tachyarrhythmia. Arrhythmias can occur in the upper chambers (atria) or the lower chambers (ventricles) of the heart.
- Atrial arrhythmia – This type is often caused by dysfunction of the sinus node, impulse generating tissue and the heart’s natural pacemaker. It can also be caused by the development of another pacemaker or circuit within the atrium (the upper chamber where blood enters the heart) that takes over the function of the sinus node.
- Atrial fibrillation – This is the most common abnormal heart rhythm disorder, when the electrical signals come from the atria at a very fast and erratic rate. The ventricles then contract in an erratic manner because of the erratic signals coming from the atria.
- Ventricular arrhythmia – This type originates from the ventricle (the lower chamber where blood is pushed out of the heart) and takes over for the natural pacemaker. Ventricular arrhythmias can be life-threatening, and immediate medical attention should generally be sought.
Some heart rhythm disorders can be inherited arrhythmias, which are based on your genes.
Arrhythmia symptoms
The effects of arrhythmia on the body are often the same whether the heartbeat is too fast, too slow or irregular. Some symptoms of arrhythmias include, but are not limited to:- Fatigue
- Lightheadedness
- Palpitations
- Weakness
The symptoms of arrhythmias may resemble other conditions, so it’s important to talk to your doctor for a diagnosis.
Causes
Certain health conditions can cause you to develop an irregular heartbeat. These conditions include:
- Changes to the heart’s structure due to an underlying condition like cardiomyopathy
- Coronary artery disease
- Diabetes
- Heart attack
- High blood pressure (hypertension)
- Overactive (hyperthyroidism) or underactive (hypothyroidism) thyroid gland
- Scarring of heart tissue due to prior heart attack
- Sleep apnea
Other factors that can cause an irregular heartbeat include:
- Being a smoker
- Drinking excessive amounts of caffeine or alcohol
- Having certain genes
- Having unmanaged stress or anxiety
- Taking certain medications and supplements, such as over-the-counter cold and allergy drugs and nutritional supplements
- Using recreational drugs
Preventing an arrhythmia
Living a heart-healthy lifestyle can help reduce your chances of developing an arrhythmia. Lifestyle modifications you can make to reduce your risk include:
- Achieving and maintaining a healthy weight
- Eating a heart-healthy diet that is high in fresh fruits, vegetables and whole grains, and low in saturated fats and cholesterol
- Getting regular exercise
- Limiting or avoiding alcoholic and caffeinated drinks
- Managing the stress and anxiety in your life using healthy coping mechanisms
- Not smoking
- Speaking with your doctor or pharmacist before taking cough and cold medications, as these can affect your heart rate
Electrophysiology study
An electrophysiology (EP) study is an invasive test of the electrical system of the heart to help diagnose an abnormal heart rhythm. A heart rhythm expert (electrophysiologist) performs this test. The electrical system of the heart is the part of the heart that coordinates the beating of the heart muscle. Entering a leg vein, the electrophysiologist positions electrode catheters (long wires) inside your heart using X-ray guidance. The electrophysiologist uses these electrode catheters to evaluate the electrical system of the heart to see if there is a problem with the heart rate going too slow (bradyarrhythmia or bradycardia) or too fast (tachyarrhythmia or tachycardia).
Conditions diagnosed
If you’re experiencing symptoms such as fainting, episodes of almost fainting, sensations of rapid heartbeats or excessively slow heartbeats, your physician may recommend an electrophysiology study. Your electrophysiologist will make a diagnosis based on the results of your study. If you are found to have a heartbeat that is too fast, you may be a candidate for catheter ablation. Your physician will also be able to determine if you are a candidate for a pacemaker or implantable cardioverter defibrillator based on the results of your electrophysiology study.
What to expect during an electrophysiology study
Preparing for your procedure
You shouldn’t eat or drink anything other than water for a period of time before the test, often starting at midnight the night before your test. Your physician will give you specific instructions on which medicines, if any, you should stop taking before the test. If you’re not given specific instructions, please take your medicines as you normally would.
On the day of your EP study, a nurse will start an intravenous (IV) line. The IV line allows the doctor to give you medicine during the test, if needed. Your nurse will also shave an area over your groin. This is where your doctor will insert the tubes (catheters) and wires during your test.
Although you’ll receive a general time for your test, you may undergo the EP study at any time during the day. The time will depend on how many patients are scheduled, how long each test takes and if there are any emergencies.
During your procedure
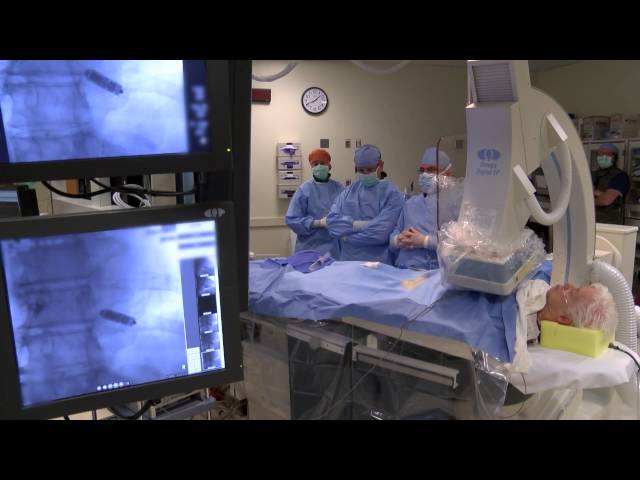
You’ll undergo the EP study while you’re sedated to a comfortable state, but you will not be under general anesthesia unless ordered by your doctor. Members of your care team will help you onto the X-ray table, and the nurses will prepare you for the procedure by placing adhesive pads on your chest and legs. A nurse will place a large sterile sheet over your body, from your neck to your toes. Your electrophysiologist will then insert catheters (flexible tubes) or pacing wires into the blood vessel in the groin area. The anesthesiologist will inject local numbing medicine so that you don’t feel any discomfort when the electrophysiologist places the catheters.
Your electrophysiologist will position the pacing catheters into the heart using X-rays to guide positioning of the catheters. These catheters allow recording and testing of your heart’s electrical system.
Your test may be brief or may last a few hours. Your electrophysiologist will do the test as quickly and as safely as possible while obtaining all of the information needed.
After your procedure
When the test is over, your electrophysiologist removes the catheters and wires and places pressure over your blood vessels to stop any bleeding. To prevent bleeding, you’ll need to be in bed and have your leg straight for about three to four hours. Your nurse will tell you when you may get up. If you need to use the bathroom during this time, please ask the nurse for help.
Your nurse will check the areas where the catheters were placed, as well as your pulse and your blood pressure several times. You’ll be able to eat and drink after your procedure. Your doctor will decide when the IV will be stopped.
Right after the test, your doctor will talk with you and your family to review the results and the plan of care for you and will relay this information to your primary care doctor.
Results of your EP study
The results of the EP study may indicate a need to implant a pacemaker to treat a slow heart rhythm, or to implant a implantable cardioverter defibrillator to treat a rapid heart rhythm from the bottom chamber of the heart.
For some patients, the EP study may reveal a rapid heart rhythm problem from the top chamber of the heart, called paroxysmal supraventricular tachycardia. Your cardiologist may recommend radiofrequency catheter ablation to manage paroxysmal supraventricular tachycardia. In this treatment, the cardiologist uses a catheter that’s positioned at the site of origin of the paroxysmal supraventricular tachycardia to deliver radiofrequency energy. The radiofrequency energy creates an irreversible lesion (injury to the tissue) in the heart to permanently eliminate the paroxysmal supraventricular tachycardia.
The initial part of the radiofrequency catheter ablation procedure is to find and map the origin of the paroxysmal supraventricular tachycardia. This process may include the use of advanced technology that allows 3D mapping of multiple heart chambers. Once your cardiologist finds the site of origin of the paroxysmal supraventricular tachycardia, they can create the ablation lesion using radiofrequency energy. Ohio State Ross Heart Hospital offers advanced ablation technology that includes use of large-tip radiofrequency catheters, cooled-tip radiofrequency catheters, pulsed-energy radiofrequency ablation and cryo-ablation energy. Radiofrequency ablation is often quite successful, with a success rate of about 96 – 98%.
Patient story: Anne Stockton
Anne thought she was having panic attacks, but it turned out to be more serious: Thanks to cardiology teams at Ross Heart Hospital, she received the diagnosis of supraventricular tachycardia (SVT) and received the treatment she needed.Why choose Ohio State for electrophysiology study?
The electrophysiology team at Ohio State Ross Heart Hospital consists of the largest group of electrophysiologists in central Ohio as well as more than 100 nursing staff members dedicated to the care of patients with heart rhythm problems. Ross Heart Hospital is also home to one of the highest volume programs in the nation.
How would you like to schedule?
Don’t have MyChart? Create an account