Back and spine trouble is one of the most common causes of chronic or debilitating pain among adults.
 Spine disorders can interfere with nearly all aspects of your life, including daily work and fun outings with friends and family. If you hope to become more active, the spine experts at The Ohio State University Wexner Medical Center can help.
Spine disorders can interfere with nearly all aspects of your life, including daily work and fun outings with friends and family. If you hope to become more active, the spine experts at The Ohio State University Wexner Medical Center can help.
Our team of orthopedic spine specialists, neurosurgeons, physical medicine and rehabilitation physicians, anesthesiologists and physical and occupational therapists are experts in treating very complex spine diseases, conditions and deformities.
With leading diagnostic tools, advanced treatments and breakthrough research, Ohio State Spine Care offers the best care for adults and children with complex spinal conditions and deformities.
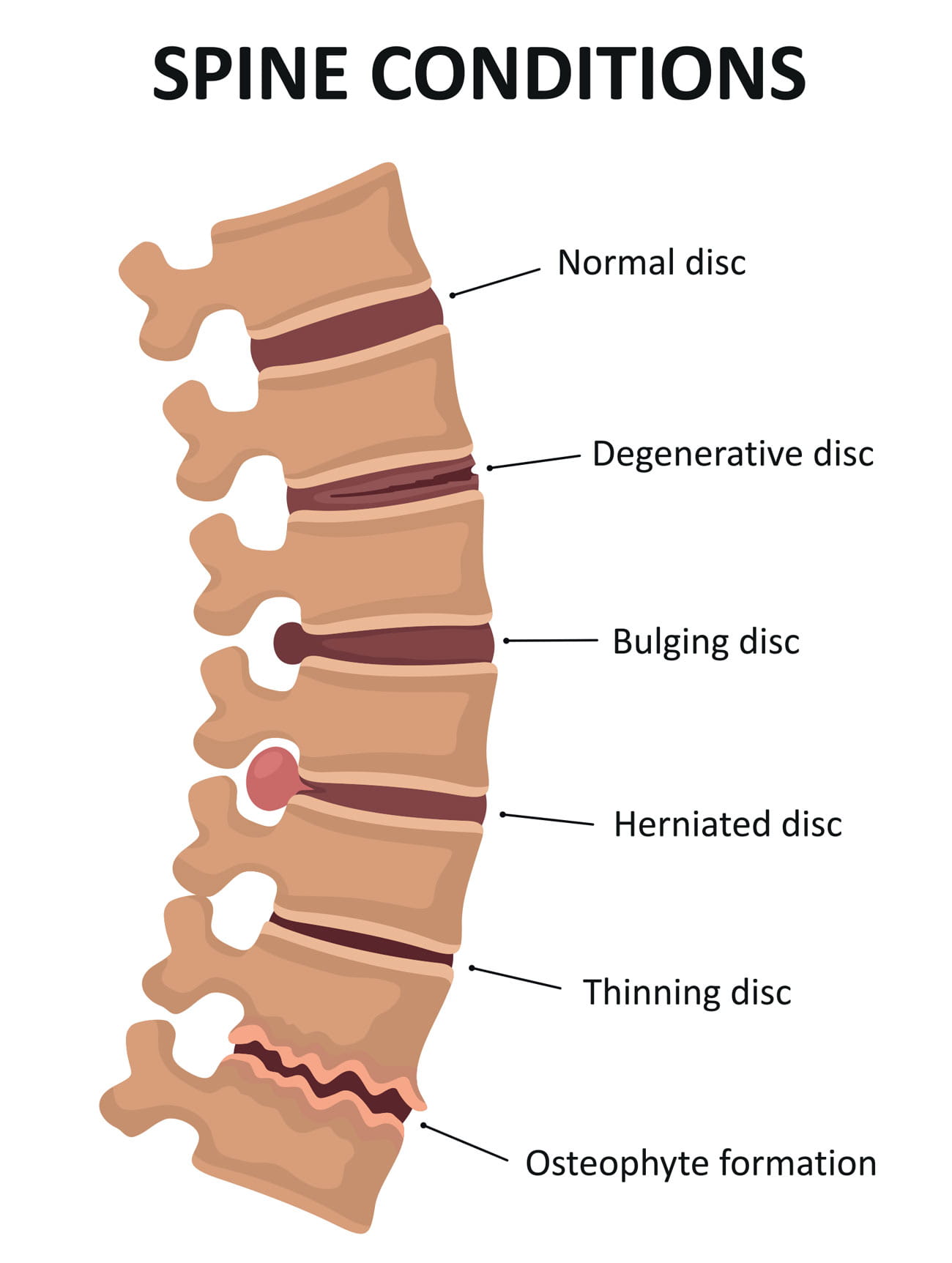
About your spine
The spinal column is your body’s main support structure. It is composed of bones, joints, muscles, ligaments, tendons, nerves and the spinal cord. Problems in the spine can be caused by injuries or underlying health problems. These issues usually don’t resolve on their own, so seeking care from experts who can provide an accurate diagnosis and the best, least invasive treatment is important.
The spine is divided into three areas of interlocking vertebrae: the neck (cervical spine), the middle (thoracic spine) and the lower (lumbar spine). The lumbar spine is the strongest part of your back and supports the weight of your upper body.
Our spine specialists in Columbus, Ohio, work closely with you to understand how your spine disorder is affecting your life and then review the best treatment option — whether it be surgical or nonsurgical.
Spine conditions we treat
Ohio State Spine Care experts treat any condition, disease or disorder that may be affecting the health of your spine. Learn more about our diagnosis and treatment of specific spine disorders:
How are spine disorders diagnosed?
Our diagnostic process includes a physical and neurological examination, which may include the use of lights or reflex hammers to assess motor, sensory and reflex skills.
Your doctor may order further imaging testing if necessary, such as an X-ray or MRI. These tests will give your physician detailed images of any deterioration or abnormality in your bones or soft tissues.
Treatment for spine disorders
Our spine specialists are committed to fully understanding your specific spine disorder and its effects on your life. Depending on your condition, your treatment plan may include nonsurgical or surgical options. At Ohio State, we always begin with nonsurgical options before recommending a more invasive treatment. Common treatment plans include:
- Lifestyle changes – smoking cessation, building strength in your back with Pilates or yoga, practicing proper posture
- Nonsurgical spine treatments – acupuncture, anti-inflammatory medications, physical therapy, spinal injections or spine orthobiologics
- Surgical treatments – decompressions surgery, herniated disc surgery, spinal fusion, spinal cord stimulation and spinal fusion
These are a few examples of the procedures our experts can perform. For a more complete list of procedures, view specific spine conditions to learn about our offerings at Ohio State.
Revision spinal surgery
We also offer revision spine surgery, also known as a second spinal surgery, at Ohio State Wexner Medical Center. This procedure may be recommended by your doctor for reasons such as:
- Failure of first spinal surgery to resolve your pain after three months of surgery
- You’re experiencing a degeneration or herniation of a disc near the area of your spine that was operated on
- An unrelated segment of your spine may develop a spine condition
Why choose Ohio State spine care for your treatment
- Ohio State Spine Care brings together the collective expertise of neurological physicians, orthopedic doctors and physical therapists who all specialize in spine disorders and injuries.
- Our team always starts with the least invasive treatment to provide you with the best result possible.
- If you need surgery, our fellowship-trained surgeons perform more complex spine surgeries here than at any other health center in central Ohio.
- We can predict whether a job or activity could injure your spine, using our biomechanical testing (studying the action of external and internal forces on the body). We’re also developing unique programs to analyze how activities and movements can stress the spine.
- You can participate in groundbreaking clinical trials through our associations with national and international spine organizations.
- Through Ohio State Spine Care Registry, we track our patients’ outcomes (including physical function and quality of life) and compare these to national and international results to help us select the most effective treatments.
Helpful Links
How would you like to schedule?
Don’t have MyChart? Create an account








